What Is a Calcified Lung Nodule?
A calcified lung nodule is a pulmonary nodule in the lungs with calcium deposits visible on imaging. Calcified pulmonary nodules are often rounded and found incidentally on a chest X-ray or computed tomography (CT) scan. Most calcified pulmonary nodules are benign and reflect old, healed inflammation, but calcification does not automatically rule out lung cancer. The right next step depends on the calcification pattern, nodule size, whether it is changing over time, and your personal risk factors.
Some patterns of calcification strongly suggest a benign cause, while others are less reassuring. Your clinician uses this information, along with your history, to decide whether the calcified pulmonary nodule can be safely observed, requires follow-up scans, or should be sampled. Solitary pulmonary nodules and small calcified lung nodules require a different approach from multiple lung nodules or large masses. CT scans are the standard imaging modality for evaluating calcified pulmonary nodules.
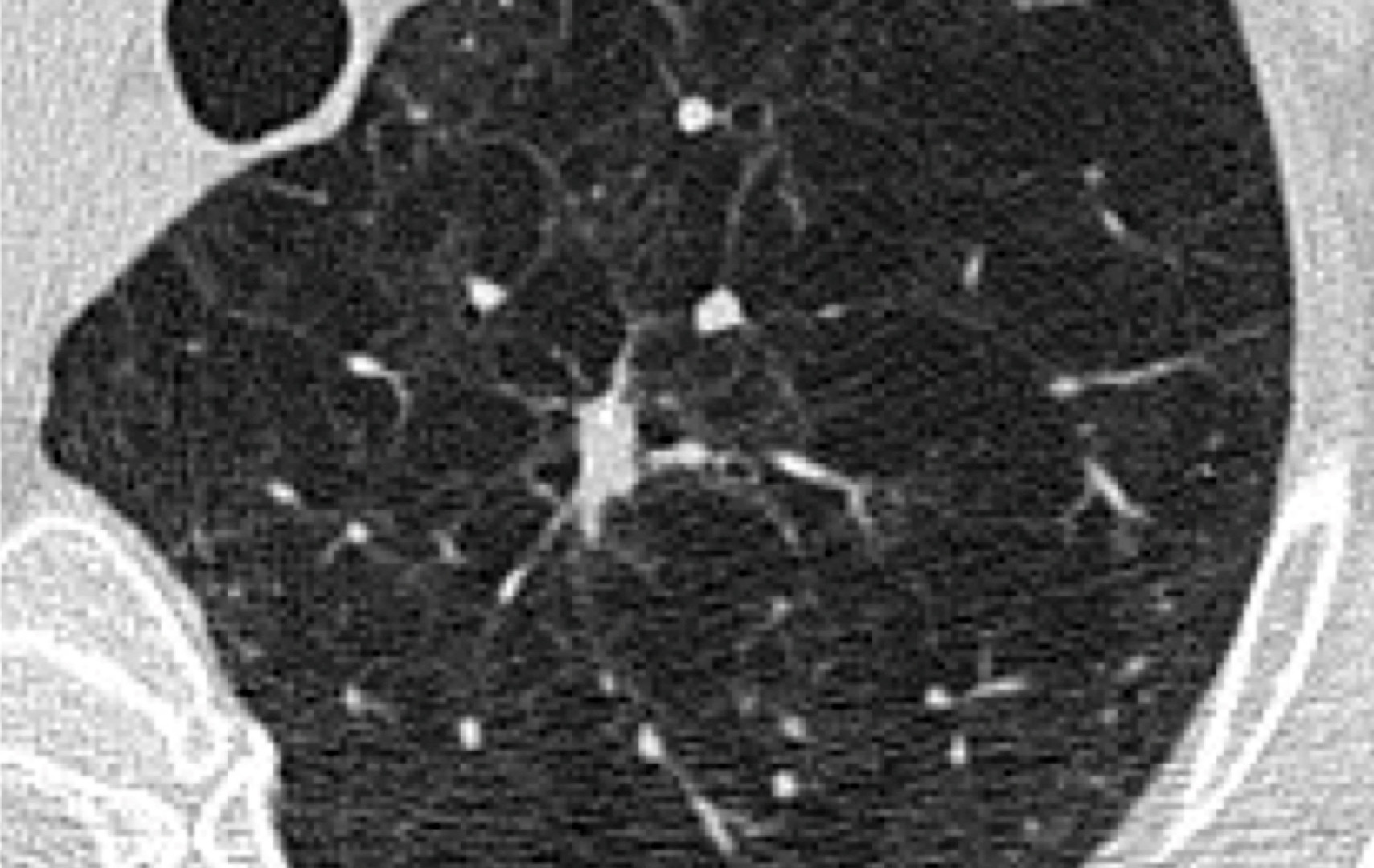
Causes of a Calcified Lung Nodule
Most calcified lung nodules are caused by an old infection or benign growths. In practice, common benign causes include calcified granulomas, which are small areas of inflammation left behind after infections such as tuberculosis or certain fungal infections. In some cases, calcified lung granulomas developed after pulmonary tuberculosis can mimic malignancy on imaging, making careful evaluation essential. It is not unusual for scans to reveal healed changes from prior infections, which may be detected during an annual health screening.
Another benign cause is a hamartoma, a common benign lung tumour, which may contain fat and calcification. A classic clue is a ‘popcorn’ calcification, and when computed tomography shows both fat and calcification within the same nodule, it strongly supports this diagnosis of a hamartoma.
Less commonly, calcified pulmonary nodules can be associated with non-infectious inflammation, such as pulmonary sarcoidosis, asbestos lung disease, or calcium deposition in metabolic conditions.
Metastatic pulmonary calcification and metastatic calcification can develop in settings such as chronic renal failure, chronic kidney disease, or metabolic lung disease, producing high attenuation pulmonary abnormalities, pulmonary calcifications, and multiple pulmonary nodular calcifications.
Calcification usually indicates a benign growth, but it does not guarantee it. Some lung cancers, including small cell lung cancer, primary lung carcinoma, primary central lung carcinoid, and bronchial carcinoid tumours, can contain calcifications from tumour necrosis or dystrophic changes.
Lung cancer can also grow around pre-existing calcified pulmonary nodules in the normal pulmonary parenchyma and lung tissue. Calcified pulmonary metastases detected on imaging may arise from primary lung tumours, pulmonary metastases from extrathoracic malignant tumours, carcinoid tumours, or lung metastases. Most calcified pulmonary metastases are from mucinous cancers. Peripheral pulmonary neoplasms, malignant mediastinal tumours, and a pulmonary artery mass are other rare causes of calcified lung nodules.
Symptoms
A calcified lung nodule usually causes no noticeable symptoms. Most lung nodules, including calcified pulmonary nodules, ground-glass nodules and indeterminate nodules are discovered incidentally on imaging done for another reason. When symptoms exist, they usually relate to the underlying cause, such as a current infection, lung cancer, inflammation, or a larger lesion affecting an airway or causing lung parenchymal involvement.
If you do have symptoms, these may include a persistent cough, breathlessness, chest discomfort, fever, or coughing up blood. Though they may not prove lung cancer, they do warrant further medical review, especially if they persist or worsen.
When to See a Lung Specialist
You should see a lung specialist if the nodule is new, changing, large, or linked with worrying symptoms or risk factors.
Many people feel anxious after reading ‘calcified nodule’ in a report, and an early specialist review can clarify what the finding likely means. Seek assessment promptly if you have coughing up blood, unexplained weight loss, persistent breathlessness, chest pain that does not settle, or a history of lung cancer.
It is also sensible to see a specialist if the report describes an indeterminate calcification pattern, irregular borders or growth compared with prior scans. Size matters too: lesions larger than 3cm are usually considered a mass and are treated as potentially malignant until proven otherwise. Your specialist will consider whether the finding could represent an extrinsic thoracic wall lesion rather than a benign calcified pulmonary nodule.

Diagnosis of a Calcified Lung Nodule
The diagnosis centres on confirming calcification patterns, comparing them with prior imaging, and assessing overall lung cancer risk.
The most useful first step is often a careful review of the CT images, not just the written report. Radiologists describe patterns of calcification and pulmonary calcifications because they provide important clues about lung nodules.
This is where the phrase ‘differentials for calcified lung nodules’ becomes practical. Your clinician considers several possibilities, including healed infection, hamartoma, inflammatory conditions, and, in less common cases, lung cancer, calcified pulmonary metastases, or pulmonary metastases from distant malignant tumours.
Your doctor will also look at your personal risk profile. Smoking history, age, exposures (such as asbestos), prior cancers, and family history can all change how aggressively a calcified pulmonary nodule should be investigated. If the nodule is new and there are no prior scans for comparison, a short-interval follow-up CT may be recommended to assess growth.
Sometimes, PET-CT is used for indeterminate pulmonary nodules on CT, but PET findings can be affected by infection or inflammation. When imaging remains uncertain, biopsy or surgical removal may be needed to establish a definitive diagnosis.
Management of Calcified Lung Nodules
The management of calcified pulmonary nodules usually consists of observation with planned follow-ups when imaging features strongly suggest a benign cause.
If the calcification pattern is clearly benign and the calcified pulmonary nodule has been stable over time, many patients do not need invasive testing. Calcified nodules with classic benign patterns of calcification, such as diffuse, central, or laminated pulmonary calcifications, can often be monitored. The safest plan often starts with checking whether older imaging is available, even if it was obtained years ago. Stability is reassuring, especially for solid lung nodules.
If your doctor suspects a healed granuloma, they may also consider your history of infections. In Singapore, past tuberculosis exposure may be relevant. Metastatic pulmonary calcification should be considered when multiple calcified lung nodules are present in patients with chronic renal failure or metabolic disorders. In some cases, additional tests are used to rule out active infection if symptoms or imaging suggest it.
If the lung nodule is indeterminate, a follow-up CT is usually the next step. The timing depends on the nodule’s size, appearance, and risk profile. The goal is to avoid unnecessary procedures without missing early lung cancer or malignant nodules.
When Surgery Is Needed
Surgery is considered when a calcified lung nodule is suspicious, growing, causing symptoms, or cannot be diagnosed safely by less invasive methods.
Most calcified nodules and calcified lung nodules do not require surgery, but there are situations in which removal is the safest path forward to establish a diagnosis or treat the lesion. Examples include calcified lung nodules, other lung nodules with concerning features, calcified nodules that enlarge over time, or cases in which biopsy of calcified pulmonary nodules yields inconclusive results.
At Neumark Lung & Chest Surgery Centre, surgery is planned with a focus on accuracy and recovery. Dr Harish Mithiran, senior consultant thoracic surgeon at Gleneagles and Mount Alvernia hospitals, uses minimally invasive approaches whenever appropriate:
- Video-Assisted Thoracoscopic Surgery (VATS) can remove a nodule and surrounding lung tissue through small incisions, often as a wedge resection or segmentectomy, and can be used to obtain a definitive diagnosis while limiting chest wall trauma.
- Robotic-Assisted Thoracic Surgery (RATS) may be helpful for precise dissection in tight spaces and for complex anatomy, including lymph node sampling when needed.
- Uniportal VATS (U-VATS) is a single-incision approach that may be suitable for selected patients and procedures, depending on the location and surgical judgment.
Not every nodule can be removed minimally invasively. Dense scarring, difficult positioning, or the need for a larger resection may require a different approach, and your surgeon will walk you through whichever method best suits your situation.
Risks and Recovery
Most patients recover well after a minimally invasive surgery for calcified nodules, but it is still an operation with real risks. Surgical risks include bleeding, infection, pneumonia, prolonged air leak, and pain. Rarely, an operation that begins minimally invasively may need to be converted to an open incision if safety requires it. Recovery varies, but many patients are walking the day after surgery and return home within a few days, depending on the extent of resection and pain control.
If the nodule is removed for diagnosis, pathology results usually guide the next step. A benign result often ends the uncertainty. If lung cancer is found, your team will promptly discuss staging and treatment planning.
How Neumark Can Help
A calcified lung nodule is often benign, but it deserves a careful, structured assessment. Neumark provides a lung specialist’s review of imaging for calcified and noncalcified pulmonary nodules, along with a risk assessment and a clear plan for follow-up or further testing when needed. Investigations and treatment can be coordinated across Gleneagles Hospital on Napier Road and Mount Alvernia Hospital on Thomson Road.
If you have been told you have a calcified lung nodule, or you want a second opinion on what your scan means, contact Neumark Lung & Chest Surgery Centre to arrange a consultation.

