What Is an Indeterminate Lung Nodule?
An indeterminate lung nodule is a small spot in the lung that is not clearly benign or clearly cancerous when it is first found. This is why the nodule is called indeterminate; imaging alone cannot immediately confirm whether it is harmless or potentially serious.
A lung nodule, also called a pulmonary nodule, is a rounded or irregular area seen on a chest scan, usually measuring up to 3 cm. These pulmonary nodules are often detected incidentally on chest X-rays or CT scans performed for other reasons. In Singapore, lung nodules are being found more frequently as chest imaging is increasingly used for health screenings, persistent coughs and post-infection assessments.
Some nodules are straightforward to interpret. A heavily calcified lung nodule that stays stable over time is usually benign and may suggest an old healed infection. A growing nodule with spiculated edges may be more concerning for lung cancer. An indeterminate lung nodule falls between these two easily categorizable extremes and needs a structured follow-up plan.
At Neumark Lung & Chest Surgery Centre, Dr Harish Mithiran takes a stepwise approach to indeterminate lung nodules, aiming to reach a precise diagnosis, avoid unnecessary invasive procedures, and identify suspicious nodules without delay.
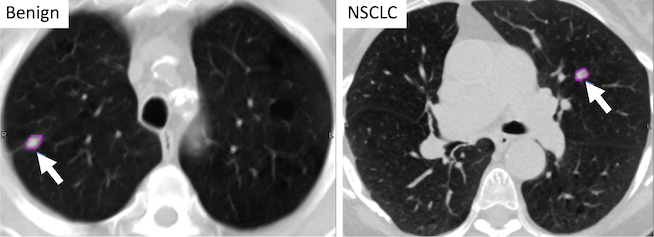
Image Source: Fred Hutch Cancer Center
Symptoms
Many lung nodules are found incidentally because they are too small to interfere with breathing or irritate the lungs. That is why people are often surprised when a scan report mentions one. When symptoms do occur, they may relate to the underlying cause rather than the nodule itself.
Possible symptoms include a persistent cough, breathlessness, chest discomfort, wheezing, coughing up blood, fatigue, or unexplained weight loss. Recurrent chest infections may also lead to imaging that reveals a nodule. However, these symptoms do not prove that the nodule is cancerous, but they do make proper evaluation more important.
When to See a Lung Specialist or Thoracic Surgeon
You should see a lung specialist when a lung nodule found on a scan is described as indeterminate, suspicious, enlarging, part-solid, or new compared with earlier imaging. It is also wise to seek review if you smoke or used to smoke, have a personal history of cancer, have a strong family history of lung cancer, or have symptoms such as coughing up blood or unexplained weight loss.
A thoracic surgeon may become involved even before surgery is certain. This can be for several reasons, such as the nodule being too hard to reach with a needle biopsy, a nodule remaining uncertain despite repeated imaging, or a nodule appearing suspicious enough that surgery may provide both diagnosis and treatment in a single procedure. Seeing the right specialist early can prevent delays and reduce diagnostic uncertainty.

Diagnosis
Diagnosing an indeterminate lung nodule means estimating the likelihood of lung cancer and deciding on the safest way to clarify it.
The first step is usually a careful review of the CT scan. The specialist assesses the CT findings, including the nodule’s size, shape, edge, density and the exact location. They also check whether there is one nodule or several, whether there are enlarged lymph nodes, and whether there are signs of infection, inflammation or scarring elsewhere in the chest. Chest X-rays may first detect an abnormality, but dedicated CT scans provide greater detail for assessing indeterminate nodules.
Comparison with older scans is one of the most useful parts of the assessment. A nodule that has not changed over time is usually less concerning than one that is growing, as malignant nodules often enlarge, while many benign nodules remain stable. That said, not all growth happens quickly. Some subsolid or ground-glass nodules change slowly and may need longer surveillance than solid nodules.
Clinical history also shapes risk. Doctors consider patient age, smoking exposure, past cancer history, family history of lung cancer, occupational exposures, immune status and symptoms. For example, a small smooth nodule in a younger non-smoker carries a different level of concern from a larger irregular nodule in an older person with a heavy smoking history.
When assessing indeterminate pulmonary nodules, clinicians also use clinical variables to accurately determine each patient’s nodule risk profile and the pretest probability of malignancy. Clinical models incorporate CT findings, such as nodule size, patient age and imaging characteristics, to determine malignancy risk and assess whether a solitary pulmonary nodule or multiple lung nodules are likely to be benign or malignant.
Further tests depend on the estimated risk. PET-CT scans may be helpful in selected cases, especially for nodules large enough to demonstrate meaningful metabolic activity. However, PET-CT scans have limitations, particularly with very small nodules and some slow-growing tumours.
A biopsy may be performed via a bronchoscopy or a CT-guided needle biopsy, depending on the nodule’s location in the lung, to help confirm malignancy or identify benign disease. In some cases, surgery may be the most reliable way to obtain a diagnosis and to rule out a malignancy.
A structured follow-up pathway is just as important as the tests themselves. One common problem with lung nodules is not a lack of technology but a lack of coordination. A patient may be told to repeat a scan in several months, yet the follow-up may be delayed, overlooked, or not clearly explained. Careful specialist oversight helps make sure the plan is appropriate and actually happens for a patient.
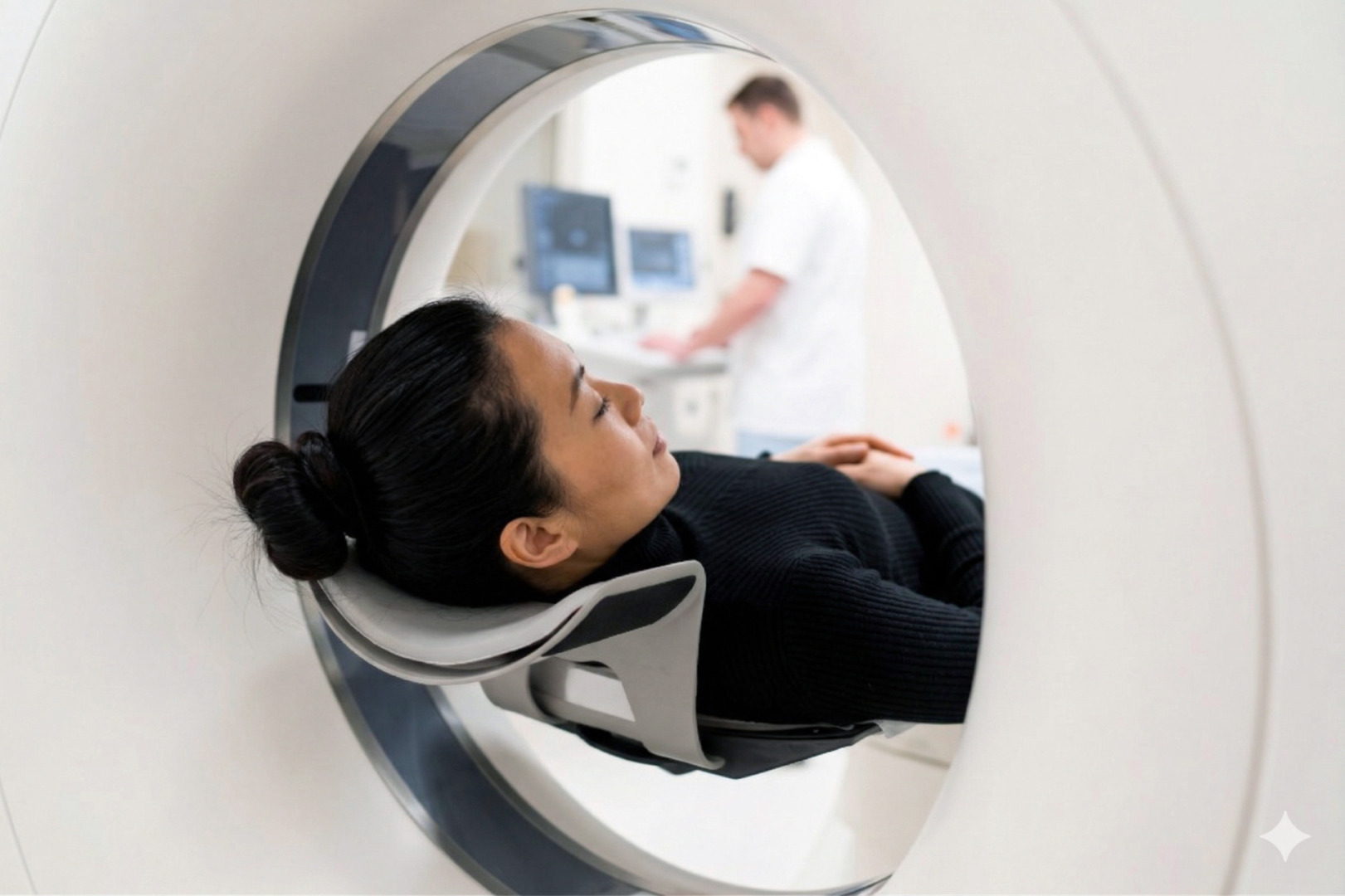
Non-Surgical Management
Many indeterminate lung nodules can be managed safely without surgery. When a pulmonary nodule is detected and appears low risk or too small for an immediate invasive procedure, active surveillance is often the best option. This means repeating CT scans at planned intervals to look for stability, resolution, or change. Surveillance is an active form of management and a viable, deliberate strategy for indeterminate lung nodules.
The follow-up interval varies. Small, low-risk solid nodules may need short- or medium-term repeat imaging, while certain subsolid nodules may require longer observations because they can progress more slowly. If the nodule remains unchanged, the level of concern often decreases. If it grows or develops a more suspicious appearance, the plan may move on to biopsy or surgery.
Non-surgical management may also include treating an underlying infection or inflammatory condition if the scan and symptoms suggest that possibility. Smoking cessation is another key part of management. It does not change the current scan, but it reduces the risk of future lung cancer and improves overall lung health. For some patients, managing anxiety is also important. Clear communication helps patients understand why surveillance may be the safest option and why immediate surgery is not always necessary.
Surgical Options
Surgery is considered when the nodule is suspicious, growing, difficult to diagnose by other means, or likely to represent an early lung cancer.
The exact operation depends on the size and location of the nodule, the person’s lung function, and the likelihood of cancer. In some cases, a wedge resection can remove the nodule with a margin of surrounding lung tissue for diagnosis. In other cases, especially when cancer is strongly suspected or confirmed, a larger anatomical resection such as segmentectomy or lobectomy may be more appropriate. Lymph node assessment may also be needed to guide staging and treatment.
Minimally invasive thoracic surgery is a major part of treatment planning at Neumark Lung & Chest Surgery Centre. Dr Harish Mithiran may use Video-Assisted Thoracoscopic Surgery, Uniportal VATS, or Robotic Thoracic Surgery where suitable. These approaches use smaller incisions than traditional open surgery and may reduce pain, shorten hospital stay, and support an earlier recovery for selected patients.
Surgery is not recommended for every case of an indeterminate lung nodule. The decision should balance the chance of cancer against the risks of an operation. For some patients, surgery offers the clearest and most efficient path to a definite diagnosis. For others, careful surveillance remains the better course for long-term safety and security.
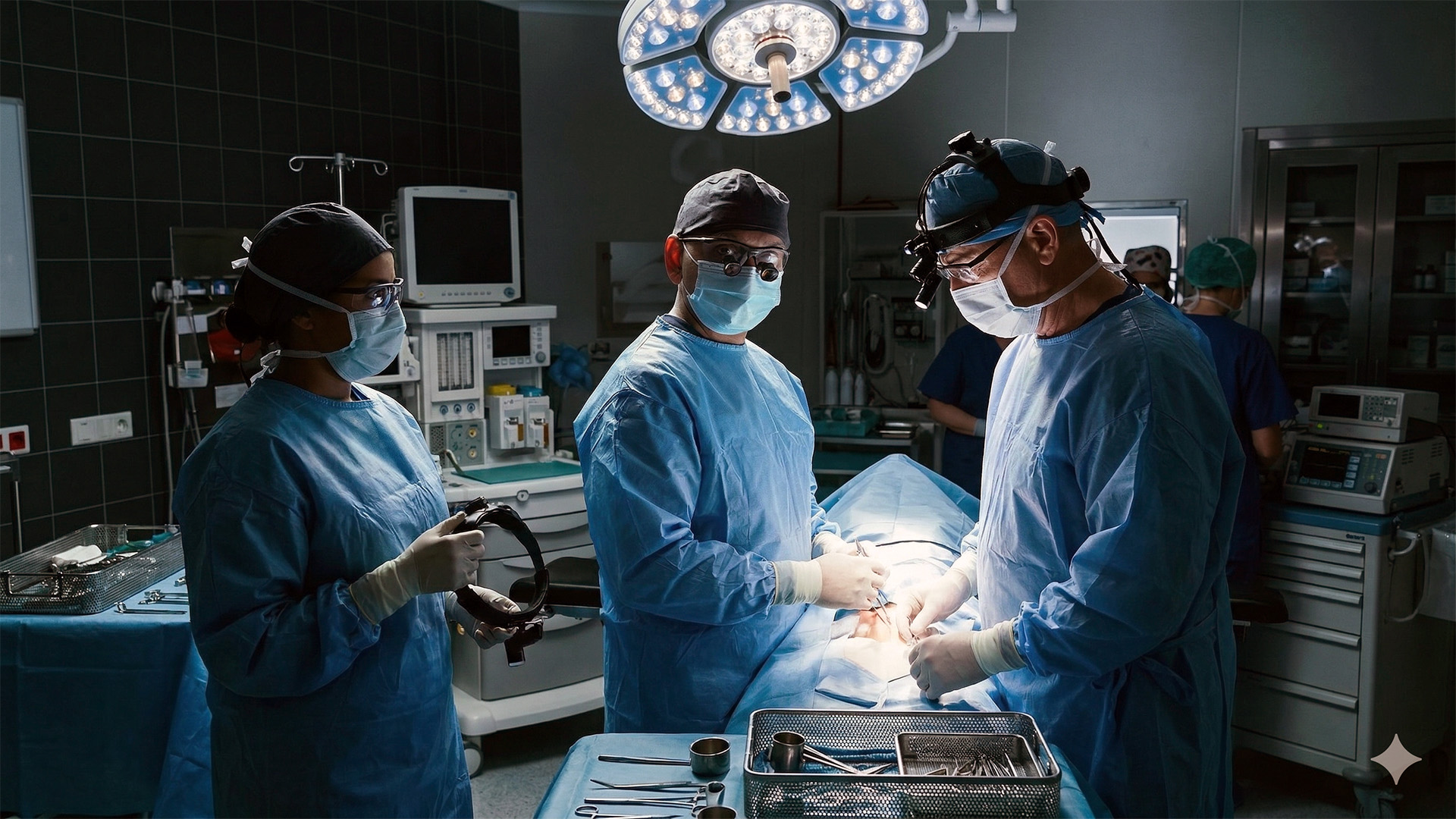
Risks and Recovery
Recovery after lung nodule surgery is usually manageable, but it requires thoughtful planning and support. The risks depend on the type of operation, the patient’s overall health, and the condition of the lungs. Possible complications include bleeding, infection, pain, air leak from the lung, pneumonia and blood clots. Patients with reduced lung reserve or other medical conditions may need closer monitoring after surgery.
Most patients are encouraged to walk, do breathing exercises, and use effective pain control to support recovery. A chest drain may be needed for a short time after lung surgery. The final pathology result is an important part of recovery, too, because it confirms whether the nodule was benign, pre-cancerous, or malignant.
Even when the nodule proves benign, the operation can still provide peace of mind by giving a definitive answer. When a cancerous lung nodule is identified, early detection can make a major difference because treatment at an earlier stage is often more effective.
How Neumark Can Help
Neumark Lung & Chest Surgery Centre can help you by turning an uncertain scan finding into a clear and personalised treatment plan. We specialise in minimally invasive thoracic surgery with a multidisciplinary approach led by Dr Harish Mithiran. For patients with an indeterminate lung nodule, we offer a careful review of the scan, a thoughtful risk assessment, and a recommendation tailored to the individual, rather than a single approach. No matter the case, the priority is the same: to reach an accurate diagnosis while protecting lung function and avoiding unnecessary treatment.
Patients often come to consultation feeling worried by an unclear scan report. A specialist like Dr Harish can help explain what the nodule means, how concerned you should be, and what should happen next. That clarity matters. An indeterminate lung nodule should not be ignored, but it should not trigger panic either. With the right evaluation, most patients can move forward with a sensible and safe plan.
If you have been told you have an indeterminate lung nodule, contact Neumark for a consultation.
FAQs about Indeterminate Lung Nodules
No, an indeterminate lung nodule is not automatically cancerous. The term only means that the scan does not yet provide sufficient evidence to confidently classify it as benign or malignant.
They are quite common, especially as CT scans are used more often for screening and for unrelated chest complaints. Many are found incidentally, and many turn out to be benign.
The follow-up period depends on the type of nodule. Solid and subsolid nodules behave differently, so some require only short-term imaging while others require surveillance over a longer time.
No, not all lung nodules need a biopsy. Many can be monitored safely with repeat CT scans if the level of concern is low.
Yes. Lung nodules can occur in people who have never smoked. Smoking increases risk, but it is not the only factor doctors consider.
Surgery is often considered when the nodule is growing, looks suspicious, cannot be diagnosed reliably by a biopsy, or is strongly suspected to be early lung cancer.

