
At Neumark Lung & Chest Surgery Centre, we offer comprehensive lung cancer screening in Singapore to detect early signs and provide the best treatment options. Early detection of lung diseases, particularly cancer, increases the chances of successful treatment.
Lung cancer is the leading cause of cancer-related deaths globally and the third most commonly diagnosed cancer for men and women in Singapore. Lung cancer remains a leading cause of cancer deaths in Singapore, and late-stage lung cancer is the leading cause of mortality among lung cancer patients. What is more startling is that 48% of non-small cell lung cancer patients in Singapore were never smokers or non-smokers.
We encourage regular health screenings and lung CT scans to help you maintain peace of mind. Singapore emphasises early lung cancer detection through Low-Dose CT (LDCT) screening for high-risk groups, including long-term smokers (50-74 years, 20+ pack-years, current/quit <15 yrs) and non-smokers with a strong family history of lung cancer. This is to improve lung cancer screening for Asian populations, aiming to catch cancers at a treatable early stage.
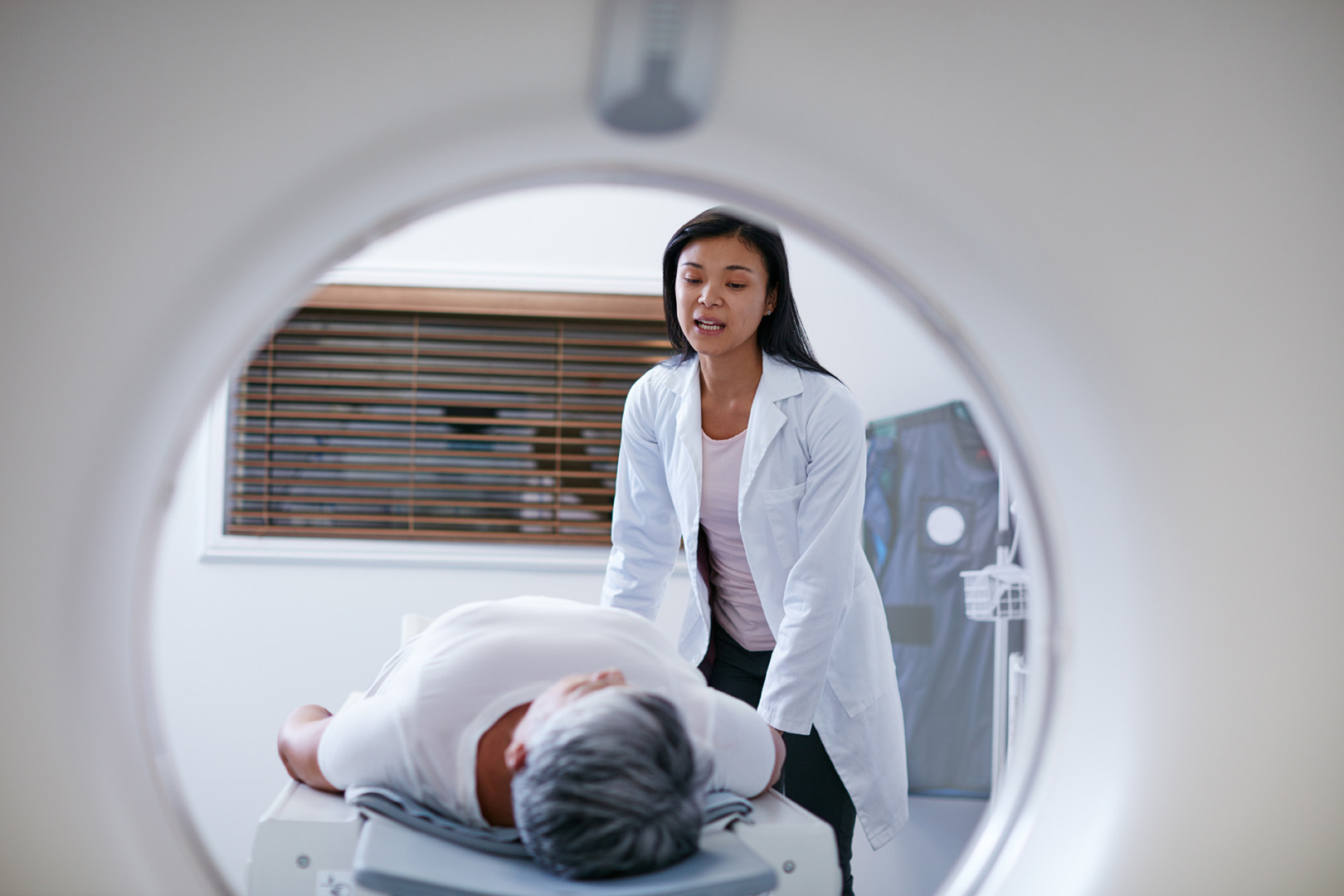
Despite modern-day advances, by the time lung cancer signs and symptoms develop, the disease has usually progressed to advanced stages, too far for curative treatments to be effective. Air pollution and secondhand smoke also contribute to the development of lung cancer. It was previously believed that all lung cancers were restricted to smokers. However, we know now that a large percentage of lung cancer cases are present in individuals who were never smokers or nonsmokers.
Lung cancers are mostly non-small cell, with a smaller percentage being small cell, which is aggressive but treatable when diagnosed early. Adenocarcinomas are the most common subtype, found in both smokers and nonsmokers. Other types include squamous cell and large cell carcinoma.

Despite rising lung cancer cases, routine screening is uncommon for non-smokers, even though a family history of lung disease or cancer significantly increases the risk. Understanding this risk is vital for prevention.
Low lung cancer screening rates are concerning, as early detection via low-dose CT (LDCT) significantly improves prognosis. LDCT is the most sensitive and specific screening test, recommended for high-risk individuals, such as smokers. Specialised LDCT scans provide detailed internal images of bones, organs, soft tissues, and blood vessels, enabling comprehensive evaluation, early detection of abnormalities, and better treatment outcomes, unlike traditional chest X-rays. The painless procedure requires no special preparation.
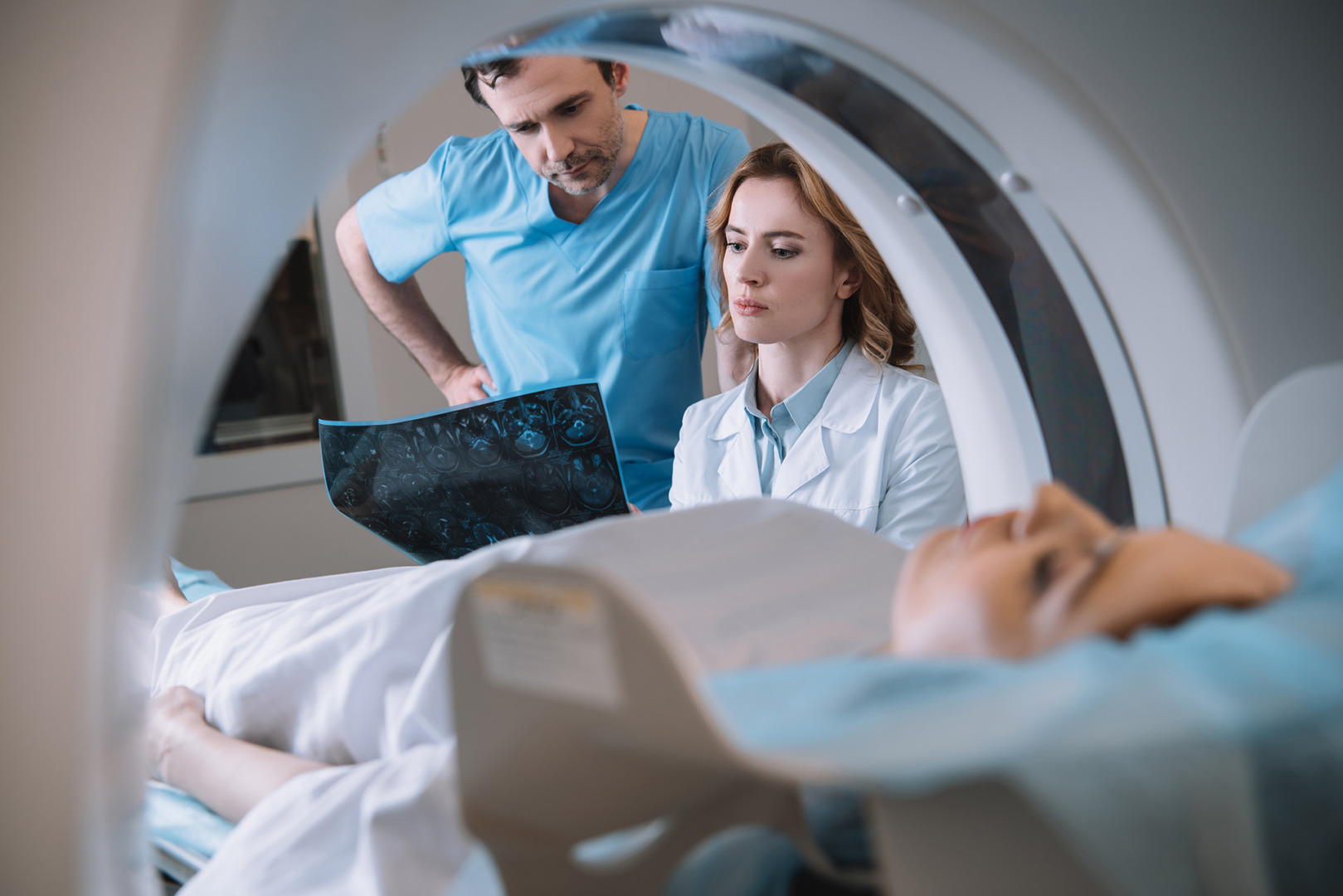
The Preventive Services Task Force recommends screening for high-risk individuals. Early detection is crucial for identifying lung abnormalities before symptoms worsen. Smoking cessation remains the best prevention strategy, a point emphasised by the World Health Organisation’s focus on cancer screening programmes.
Advances such as targeted and radiation therapy have improved outcomes, making early screening crucial for detecting treatable early-stage diseases. CT scans also identify other lung conditions (e.g. pneumonia, pulmonary fibrosis, tuberculosis) and blood vessel abnormalities (e.g. aneurysms, clots). Blood tests and biopsies further aid management.
Consult a thoracic surgeon to interpret your screening results to determine the necessary follow-up steps.
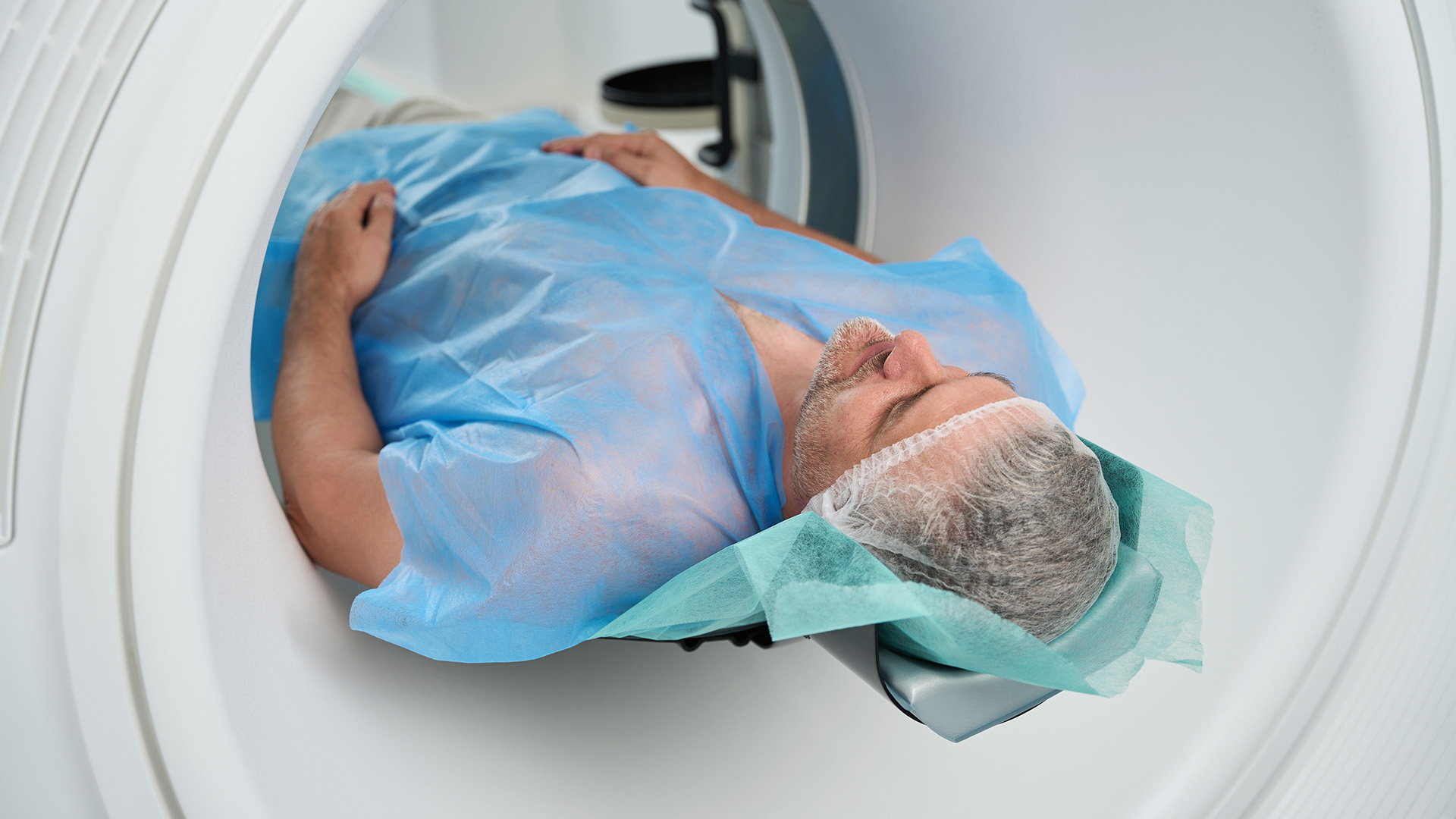
As there are no symptoms of lung cancer in its early stages, lung screening and lung cancer screening to detect any abnormalities is essential for everyone, especially those at high risk of developing lung cancer.
The Neumark Lung screening programme at our lung cancer treatment centre offers a range of lung check-ups, screenings, and diagnostic tests to detect lung cancer, including small-cell lung cancer and other types. This lung screening programme is designed to detect early-stage lung cancer.
At the core of Neumark’s comprehensive lung cancer screening programme is a 10-minute low-dose computed tomography (LDCT) imaging exam, cardiopulmonary exercise testing, and pulmonary functional testing, followed by a thorough review of your results with our thoracic surgeons, specialists in lung conditions. This dose computed tomography LDCT approach is the gold standard for lung cancer screening.
The screening tool is highly effective at identifying abnormalities in the lungs that may be indicative of cancer cells and can detect early signs of lung cancer:
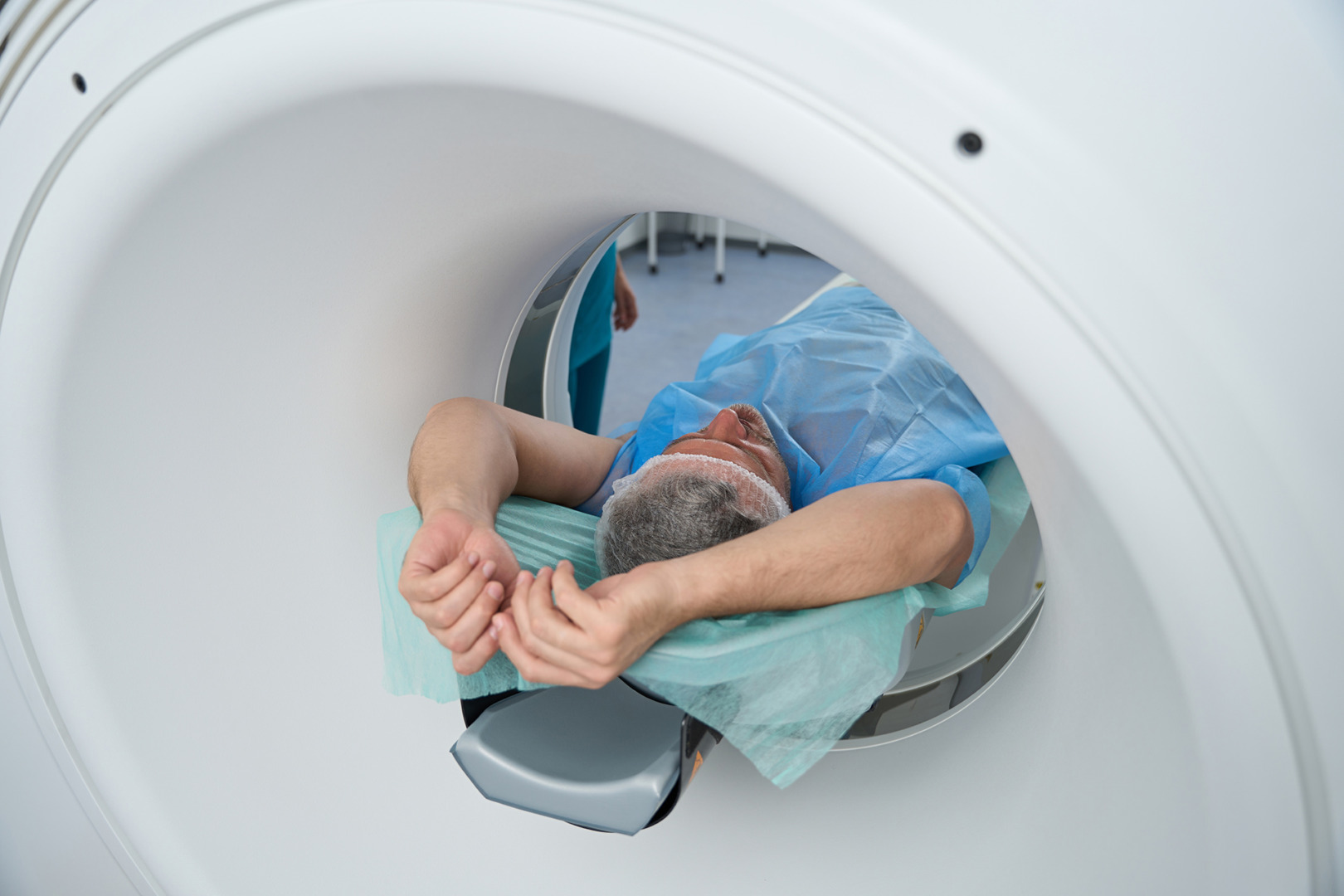
Cardiopulmonary Exercise Testing (CPET) is a vital assessment tool for thoracic surgeons to evaluate a patient’s heart and lung function during exercise, ensuring normal lung function, optimal surgical readiness and personalised treatment plans for improved health and treatment outcomes. This helps assess lung cancer risk.

Pulmonary Function Tests (PFTs) are comprehensive assessments that measure lung capacity and efficiency, enabling healthcare professionals to diagnose respiratory conditions, evaluate the effectiveness of cancer treatment, and plan the appropriate surgical interventions.

Neumark’s multidisciplinary team works alongside the National Cancer Centre Singapore and the National University Hospital:
Lung cancer screening helps Neumark surgeons detect and remove suspicious or cancerous tissue early, reducing the risk of future cancer development and mortality. If abnormalities are found, additional follow-up or blood tests may be necessary. Regular screening offers the best protection for high-risk individuals.

Neumark Lung and Chest Surgery Centre offers lung cancer screening assessments with specialist guidance at two convenient hospital locations in Singapore:
Gleneagles Hospital (Napier Road)
Nearest MRT: Napier (TE12)
Mount Alvernia Hospital (Thomson Road)
Nearest MRT: Caldecott (CC17/TE9) or Marymount (CC16)
If you have risk factors such as a smoking history, or you have been advised to consider low-dose CT screening, our team will guide you through suitability, next steps, and follow-up planning, including a review of your scan results and any incidental findings, such as lung nodules.
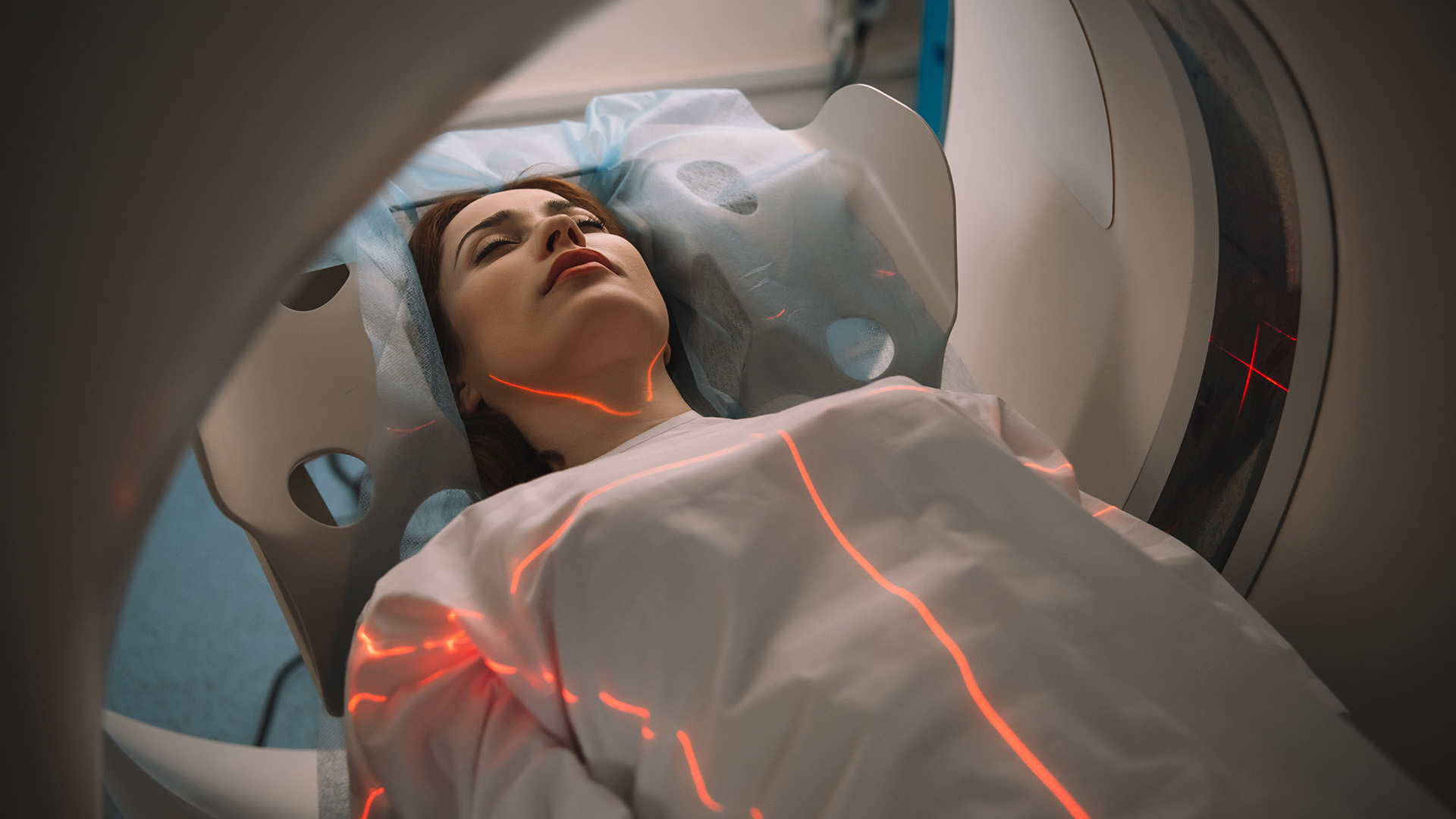
Low-dose computed tomography (LDCT) is the gold-standard imaging for early lung cancer detection in high-risk individuals and the general population. This noninvasive, quick (10-15 min) CT chest scan uses spiral X-rays to create detailed 3D images, revealing early-stage lung nodules that traditional chest X-rays miss.
Early identification of smaller tumours through LDCT significantly increases the likelihood of diagnosis before metastasis, improving survival and expanding treatment options such as targeted and radiation therapy. No injections, dyes, or pills are needed. Screening is conducted at Gleneagles or Mount Alvernia hospitals in Singapore, in accordance with international guidelines.
Neumark’s thoracic surgeons review the results with the patient. LDCT is an early detection tool, not a definitive diagnosis; abnormalities or signs of cancer may require further testing to confirm a diagnosis.
Preparing for a lung check-up is an essential step to ensure your CT low-dose lung cancer screening is as accurate and effective as possible. Our clinical team will provide you with specific instructions tailored to your individual needs and the type of scan you are having. For most low-dose CT scans used in lung cancer screening, preparation is straightforward. However, there are a few key points to consider.
If your CT chest scan requires contrast dye, you may need to fast for 4-6 hours. Inform your doctor about all medications, allergies (especially to iodine or contrast materials), and any history of lung cancer, kidney problems, or diabetes, as these may affect the scan’s safety and approach. Medication may be prescribed to reduce the risk of an allergic reaction to the dye. Also, report any environmental exposure to harmful chemicals or air pollution.

Before the scan, remove any metal objects, such as jewellery or glasses, and you will be asked to wear a gown. Alert your doctor if you are pregnant or suspect you might be, as this impacts the decision to proceed or use contrast dye.
On the day of the screening, you will lie on a table that slides into the doughnut-shaped CT scanner. The scan is quick and painless, usually taking less than 15 minutes. You may be asked to hold your breath briefly for clear images. A technologist will operate the machine from a separate room but will be able to see, hear and communicate with you.
Afterwards, you can typically resume normal activities. If contrast dye was used, you will have to drink plenty of water to help flush it out.
Your doctor will review the images and discuss the results, including next steps if abnormalities are found.
If you have questions about the scan, radiation, or procedure, speak with your doctor. Understanding the lung cancer CT scan helps reduce anxiety. Following preparation guidelines and communicating openly ensures an effective, stress-free screening.
A comprehensive check-up, which may include a physical exam, discussion of symptoms and risk factors (including family history), lung function tests, blood tests and CT scans, can detect cancer early. High-risk individuals (smokers, those exposed to secondhand smoke or air pollution, or with a family history of lung disease/cancer) may need annual check-ups; others less frequently. The Singapore Cancer Registry data guides screening recommendations.
At Neumark Lung & Chest Surgical Centre, lung cancer patients receive expert care from Dr Harish Mithiran, director and senior consultant thoracic surgeon at Gleneagles and Mount Alvernia hospitals in Singapore. Treatment focuses on improved outcomes through personalised coordination and groundbreaking, minimally invasive procedures, such as robotic or uniportal video-assisted thoracoscopic surgery, aiming for successful treatment in all cases.
A low-dose CT scan for lung cancer screening in Singapore costs $400 before GST. For appointments or further information about the lung cancer screening process, please contact the team at Neumark Lung & Chest Surgery Centre. Remember, early detection of lung cancer through cancer screening saves lives.
Insurance may cover the cost of lung health tests and lung cancer screening for most patients with lung cancer who meet the screening criteria. Patients should check with their insurance provider to determine their coverage for this type of procedure by checking with your insurance panel.
A CT scan screening for smokers is a low-dose computed tomography (CT) scan specifically designed to detect lung cancer early and identify early signs of lung cancer in current or former smokers who are at high risk of developing lung cancer. Quitting smoking and smoking cessation significantly reduce lung cancer risk even after years of cigarette smoking.
A dose of computed tomography LDCT lung cancer screening uses about 90% less radiation than a standard CT scan, while still providing detailed images of the lungs to detect lung cancer. This dose computed tomography LDCT and low dose computed tomography approach is preferred for lung cancer screening in Singapore.
If contrast material is to be used, you may be asked to remove metal objects and refrain from eating or drinking for a few hours before the scan. The scan typically takes only a few minutes, but the appointment usually lasts around 30 minutes. Discuss your family history of lung cancer and history of lung cancer in relatives, and any environmental exposure to harmful chemicals, air pollution, or secondhand smoke with your doctor.
DISCLAIMER: The information provided on this website is for general informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. The use of this website does not create a doctor-patient relationship and no medical advice should be inferred or assumed. It is the user’s sole responsibility to seek the advice of their healthcare professionals for any medical concerns they may have and the user should not disregard, or delay, prompt medical advice for any such condition.
Read our latest insights on lung diseases and chest conditions, including prevention tactics, treatments, and more.
Gleneagles Medical Centre
6 Napier Road
#02-09 Gleneagles Medical Centre
Singapore 258499
Mount Alvernia Hospital
820 Thomson Road
#06-07 Medical Centre A
Singapore 574623