What Is a Ground-Glass Nodule?
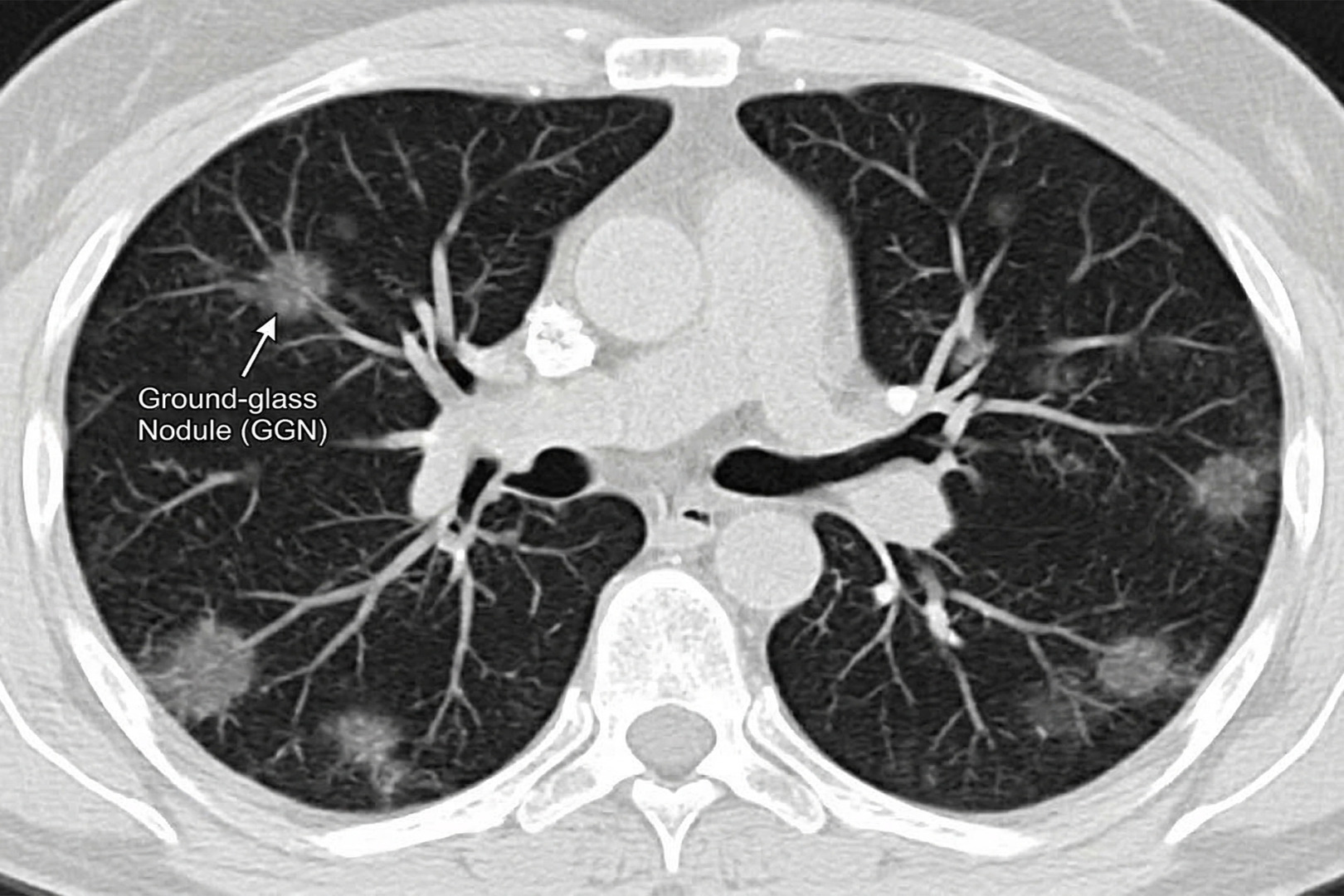
A ground-glass nodule (GGN), sometimes called a ‘ground-glass opacity’, is a faint, hazy area on a CT scan of the lungs that still allows normal lung markings to be seen through it. It is important to note that this is a description of how the nodule appears on imaging, not a diagnosis in itself.
Seeing a ground-glass nodule on a report can be worrisome, but most are not an emergency. Many are caused by temporary inflammation or infection and may disappear on repeat scanning. Others persist, and a small number represent very early lung cancer. The key questions are whether the nodule is truly persistent, whether it has any solid component, and whether it is growing.
A computed tomography (CT) scan is the best test for characterising ground-glass nodules and guiding the next steps. In Singapore, more people now have CT scans, including low-dose CT screening, meaning ground-glass nodules are being found more frequently, sometimes even when patients feel completely well. At Neumark Lung & Chest Surgery Centre, Dr Harish Mithiran reviews the images in detail and recommends a clear plan that may include a short-interval follow-up CT, structured surveillance, or further testing as needed.
Lung specialists often describe three patterns of pulmonary lesions:
- Pure ground-glass nodules (ground-glass opacity, nonsolid nodules) are entirely hazy and do not obscure underlying bronchial structures.
- A part-solid nodule, which has both ground-glass opacity and solid components, is like an indeterminate lung nodule.
- A solid, calcified nodule which blocks lung markings more completely.
This distinction matters because part-solid nodules with solid components are more likely to represent early-stage lung cancer or lung adenocarcinoma than a pure ground-glass nodule of the same size. In the lung adenocarcinoma spectrum, ground-glass opacity may represent atypical adenomatous hyperplasia, minimally invasive adenocarcinoma, or invasive adenocarcinoma.
People also ask about the life expectancy of ground-glass nodules. A ground-glass nodule is a scan finding, not a clinical diagnosis in and of itself. Many are benign lesions. When a persistent ground-glass opacity represents early-stage lung cancer, it often grows slowly and has a favourable prognosis when managed early. Early diagnosis through CT screening improves outcomes.
Causes of Ground-Glass Nodules
Common causes of a ground-glass opacity include:
- Temporary inflammation or infection
- Viral infections and mild pneumonias causing ground-glass opacity changes that resolve
- Immune cells causing transient pulmonary ground-glass changes
- Small areas of bleeding into the lung, sometimes caused by severe coughing or blood-thinning medications
- Immune cell responses that create lung nodules and pulmonary lesions
- Scarring of lung nodules and other lung nodules, focal interstitial fibrosis, or healing after infection
If you have more than one finding, it’s normal to wonder about the reasons for multiple spots or cloudy areas in your lungs. Having several nodules can be due to infections, inflammation, or other widespread lung diseases. Occasionally, multiple ground-glass nodules can be an early sign of multiple small lung cancers. The best way to tell them apart is to look at the pattern and how they change over time on follow-up scans.

Symptoms
A ground-glass opacity is commonly discovered during lung cancer screening, an incidental health screening CT scan, a preoperative scan, or evaluation of chest discomfort. Ground-glass nodule symptoms are usually absent, and most people feel completely well when the nodule is found.
If symptoms are present, they usually relate to the underlying cause rather than the nodule itself. Lung infections or inflammation may cause cough, fever, breathlessness, or chest tightness. Lung cancer can cause symptoms, but early ground-glass nodules often cause none.
When to See a Lung Specialist
You should see a lung specialist when a ground-glass nodule is persistent, enlarging, has solid components, or occurs in someone with higher-risk factors. Your doctor may recommend a repeat CT scan.
Specialist review by a thoracic surgeon is helpful if:
- The report suggests part-solid nodules with solid components or part-solid nodules showing growth.
- You have a personal history of lung cancer or other cancer.
- You have a significant smoking history, asbestos exposure, or a strong family history of lung cancer.
- The nodule is new, and there are no prior imaging scans for comparison. You feel anxious and want a clear plan rather than uncertainty.
In Singapore, incidental pulmonary nodules and small pulmonary nodules detected on CT screening are increasingly common as more people undergo lung cancer screenings. The results determine whether follow-up action is needed.
Diagnosis of Ground-Glass Lung Nodules
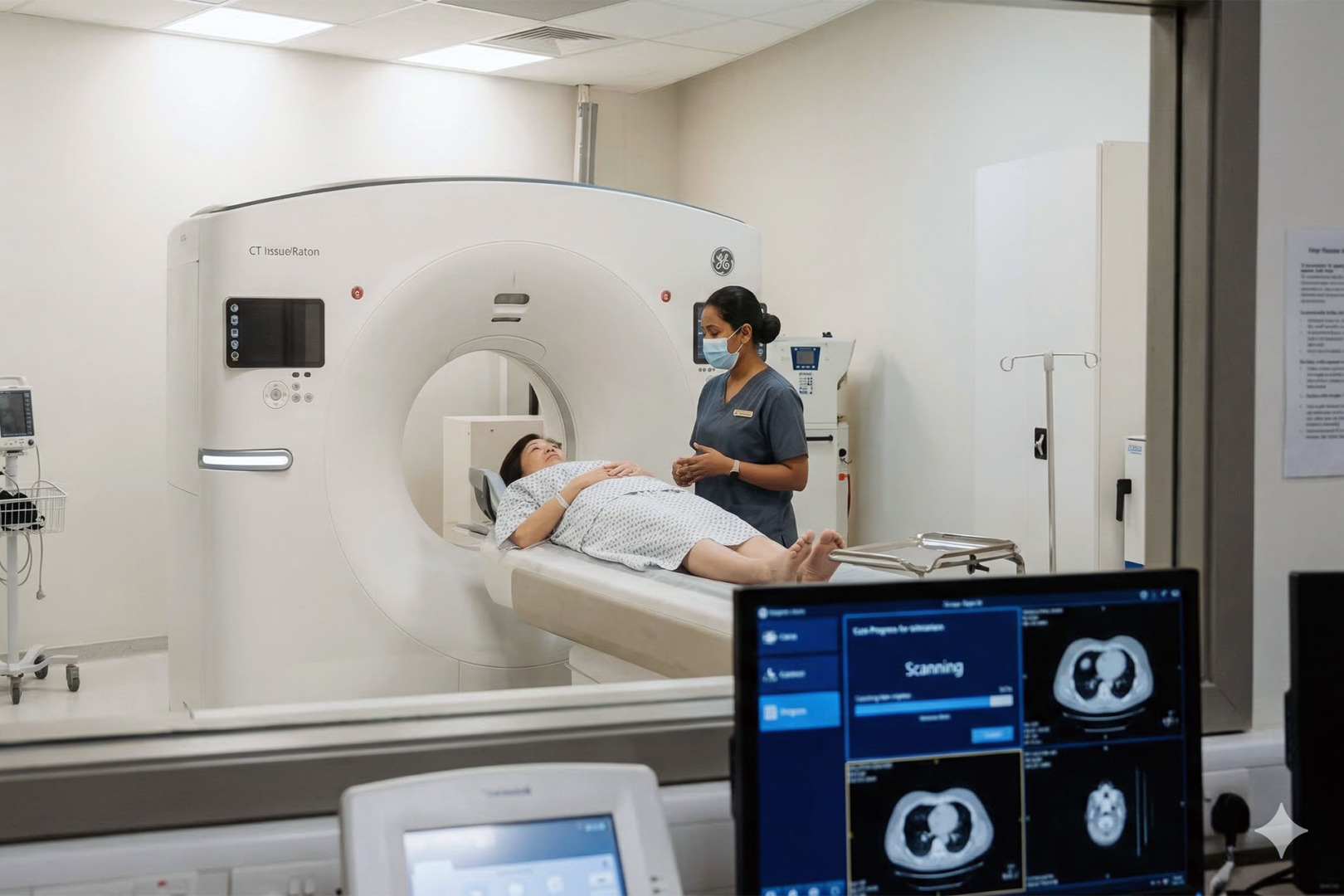
Diagnosis of a ground-glass nodule relies on the careful interpretation of computed tomography, comparison with prior CT scans, and, in some cases, tissue sampling. The key diagnostic work for a ground-glass opacity focuses on imaging features such as size, shape, margins, solid components, and the presence of part-solid versus nonsolid nodules.
A lung specialist will usually start by answering four questions:
- Is it persistent, or could it be temporary inflammation?
- Is it pure ground-glass opacity, or part solid nodules with solid components?
- Is it stable, growing, or developing solid components?
- Do your personal risk factors raise concern?
The quality of the CT scan is important. Thin CT ‘slices’ help lung doctors accurately measure tiny lung spots and see any subtle solid parts within them. If older CT scans are available, comparing them can be helpful and reassuring.
A PET-CT scan is sometimes considered, but ground-glass nodules may not appear as brightly (‘PET-avid’) as solid nodules. Therefore, a negative PET scan doesn’t always rule out early lung cancer. This is why watching the appearance and behaviour of the nodules on multiple CT scans over time is often more useful. Lung function tests might be ordered before surgery is considered.
Research into common lung cancers shows that genetic alterations (such as EGFR mutations or other ‘driver gene’ mutations) affect how the cancer behaves. Information about these molecular characteristics, such as EGFR status and blood test results, helps doctors complement imaging findings to enable an early diagnosis of more serious lesions. These clinical and genetic insights help predict the nodule’s behaviour, the risk of lymph node spread, and overall patient outcomes.
If the nodule looks concerning, your clinical team may consider a biopsy. However, a biopsy of small pulmonary nodules and ground-glass nodules GGNs can be technically challenging and may not always provide a definitive answer. In selected cases, surgeons may recommend surgical resection of the nodule as both diagnosis and treatment, particularly if the likelihood of adenocarcinoma is high and the nodule is in a favourable location.
Management of Ground-Glass Lung Nodules
The clinical management of ground-glass nodules is usually watchful waiting with planned CT follow-ups, unless imaging features suggest a higher risk.
If a ground-glass opacity disappears on follow-up, it is likely related to an infection or inflammation. If it persists as a ground-glass opacity but remains stable, your doctor may recommend periodic CT scans to monitor for growth or the development of solid components. The biological behaviour of pulmonary GGNs varies: some remain indolent, while others develop invasive lesions or progress to invasive adenocarcinoma.
Management of ground-glass nodules is guided by:
- Persistence on repeat imaging scans
- Size, imaging features, and morphological features
- Presence, size, and change in solid components
- Growth trend, biological behaviour, and imaging features reflecting biological behaviour
- Your risk factors and preferences
Importantly, if you smoke, stopping reduces the future risk of complications in your lungs.
When Surgery Is Needed
Surgical resection is considered when a ground-glass nodule is persistent and suspicious, especially if it grows or develops solid components. Not every ground-glass opacity requires surgical resection, and many will never need an operation. Surgical resection becomes more relevant when the balance shifts towards a meaningful chance of early-stage lung cancer or lung adenocarcinoma, and when surgical resection could be curative.
Common situations where surgical resection may be discussed include:
- Persistent part solid nodules, especially if the solid components increase.
- A pure ground-glass nodule that enlarges over time.
- A nodule that remains indeterminate after reasonable follow-up, where uncertainty is affecting quality of life.
If a patient is healthy enough for surgery and removing the nodule is likely to maintain good lung function while providing a definitive diagnosis of lung adenocarcinoma, surgical resection is considered.
At Neumark, surgical approaches and decisions are made with input from various specialists, always prioritising the preservation of healthy lung tissue. Surgical removal options include a wedge resection (taking out a small, wedge-shaped piece), a segmentectomy (removing a segment of the lung), or a lobectomy (removing an entire lobe of the lung). The choice depends on the nodule’s location, whether it has solid parts, and the level of concern. For many small, early-stage lesions with a good outlook, a limited surgery can be sufficient for early lung cancer. However, the exact procedure is determined by the need to ensure complete cancer removal, clear margins (a rim of healthy tissue around the cancer), the risk of cancer spreading to lymph nodes, and a proper assessment of those lymph nodes.
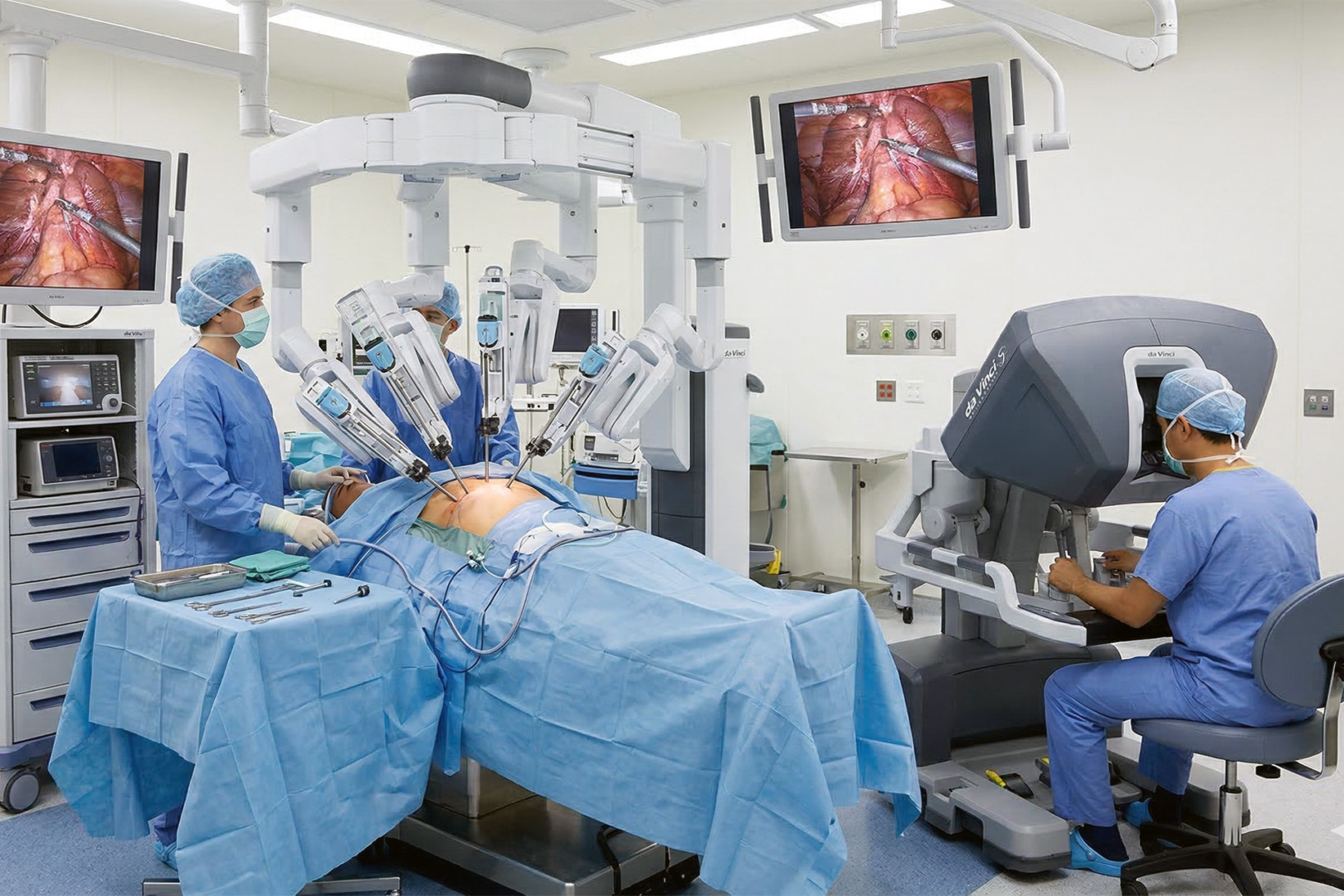
The presence of solid components within the nodule is a key factor in planning the surgery. Modern surgical techniques include Video-Assisted Thoracoscopic Surgery (VATS), robotic-assisted surgery (RATS), and uniportal VATS (U-VATS), all of which are minimally invasive.
Risks and Recovery
Most patients recover well after a minimally invasive surgical resection for a ground-glass nodule, but all surgery carries risks and requires a realistic recovery plan. Potential risks include bleeding, infection and pneumonia.
The recovery varies by the extent of surgical resection. Hospital stays are often a few days for minimally invasive procedures.
Pathology results guide the next steps. If the nodule is benign, follow-up may end or continue only briefly for routine check-ups. If it represents early-stage lung cancer, lung adenocarcinoma or invasive adenocarcinoma, your team will discuss staging, lymph node metastasis findings, and whether any additional treatment is needed. Early diagnosis of lung adenocarcinoma in the ground-glass spectrum often yields a favourable prognosis and good clinical outcomes with surgical resection alone.
How Neumark Can Help
A ground-glass nodule is best managed with careful imaging review, clear follow-up, and timely surgical resection when the risk increases. Neumark provides structured clinical management led by Dr Harish Mithiran, senior consultant thoracic surgeon, with care coordinated at Gleneagles Hospital on Napier Road and Mount Alvernia Hospital on Thomson Road. The focus is on the accurate interpretation of computed tomography findings, imaging features, and clinical significance; CT screening and ongoing CT screening; and minimally invasive surgical resection options when surgery is indicated.
If you have been told you have a ground-glass nodule, or you are unsure what your CT report means, contact Neumark Lung & Chest Surgery Centre to book a consultation and get clear answers and a management plan you can trust.

