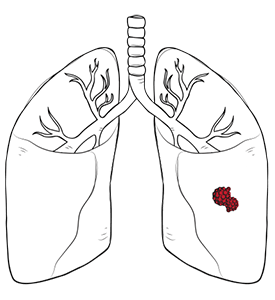
Thymoma refers to tumours that arise from the epithelial cells of the thymus gland, a small gland in the lymphatic system responsible for producing and maturing T cells (also known as white blood cells). The thymus gland contains various cell types, including epithelial cells that can give rise to epithelial tumours. Thymomas can be benign or malignant: benign thymomas grow slowly and stay within the thymus gland; malignant thymomas contain cancer cells that can invade surrounding tissues and metastasise to other parts of the body.
Thymomas are often confused with thymic carcinomas. Both arise from epithelial cells of the thymus gland, but thymic carcinomas are more aggressive and more likely to spread, leading to a poorer prognosis.
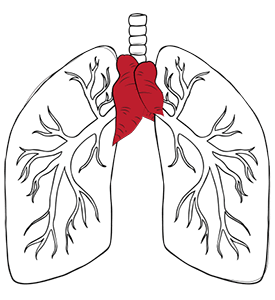
Yes, thymoma is a rare thymic cancer that arises from the epithelial cells of the thymus gland, a small but vital organ located behind the breastbone. The thymus gland plays a major role in the immune system by producing T cells that help the body’s natural defences fight cancer and infections.
Thymoma grows more slowly and spreads less often than other rare cancers. That does not mean it is not dangerous. In some cases, cancer cells can spread to the lining of the heart and lungs, or to other tissues in the body.
Thymoma and myasthenia gravis, an autoimmune condition, are closely linked, making it particularly challenging to treat. Myasthenia gravis affects almost half of all cancer patients with thymoma. Cancer treatments often require addressing both the cancer cells and the complications of the immune system.
Symptoms of thymoma may not appear until the thymic tumour grows. In many cases, thymomas and thymic carcinomas are discovered incidentally during imaging tests. When symptoms of thymoma do appear, they can include:
These cancer symptoms develop gradually as the growing tumour presses on nearby organs in the chest cavity.
In some cases, thymoma can cause paraneoplastic syndromes, conditions resulting from the tumour’s effects on the immune system. The most common is myasthenia gravis, a neuromuscular disorder characterised by muscle weakness, drooping eyelids and difficulty swallowing. Other associated conditions include Good syndrome, pure red cell aplasia, and hypogammaglobulinaemia, which causes frequent infections.
The causes of thymoma are not well understood, but genetic mutations and immune system dysfunction are thought to be involved. A medical history of myasthenia gravis or autoimmune disorders carries an increased risk. Importantly, thymoma and thymic carcinoma can affect cancer patients at any age.
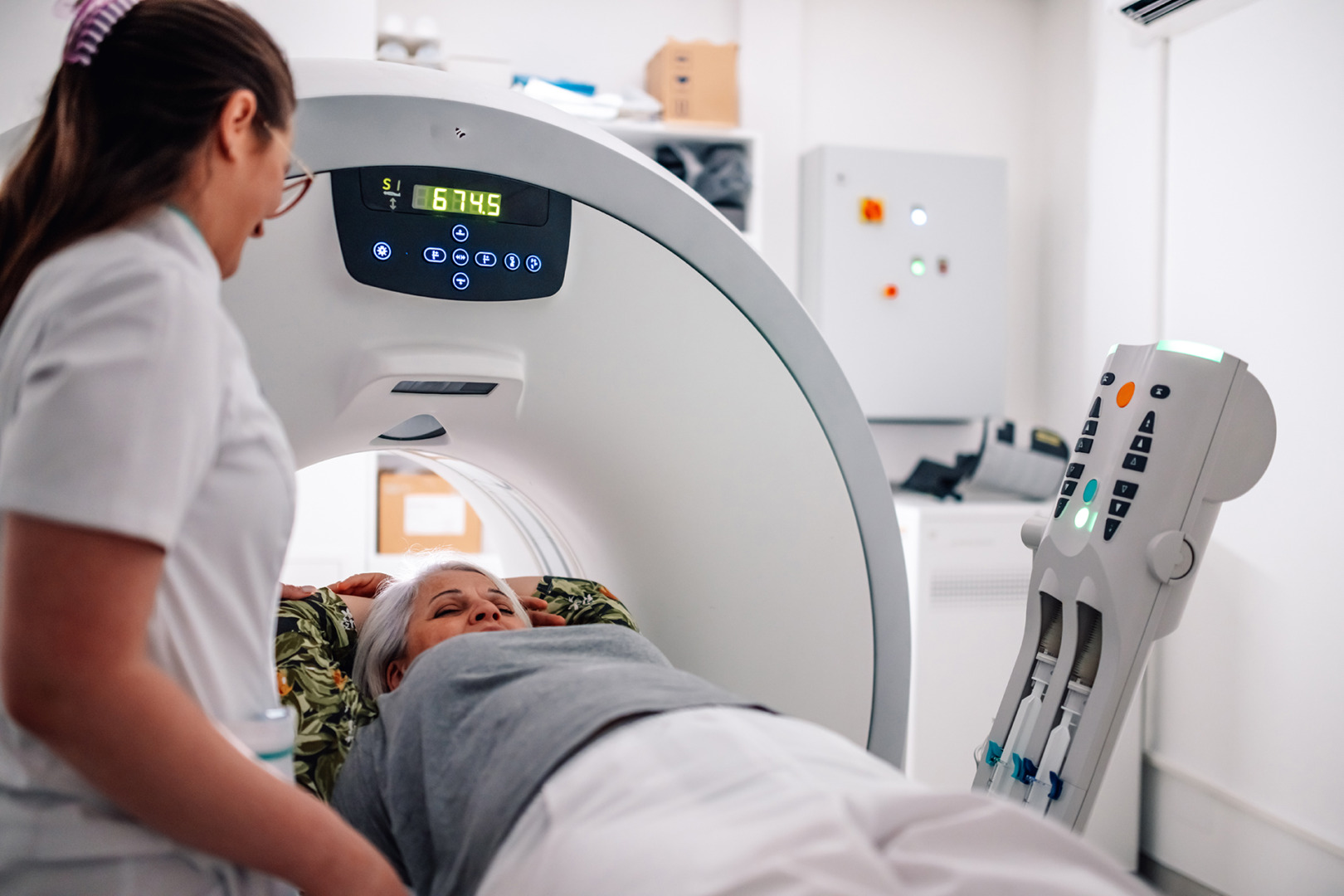
Thymoma diagnosis starts with a thorough workup, often following an inadvertent discovery on radiology imaging, such as a chest X-ray or imaging findings. Thymoma radiology, such as CT scans, shows a characteristic anterior mediastinal mass, while MRI provides detailed information on the tumour’s relationship to surrounding structures. Careful evaluation of the primary tumour, mediastinal pleura and lymph nodes during imaging and staging is crucial for accurate diagnosis and cancer staging.
If a thymoma or thymic carcinoma is suspected, a biopsy may be performed to confirm the diagnosis. A tissue sample is typically obtained via a CT-guided biopsy or surgical sampling to determine whether tumour cells and cancer cells are present, and if healthy cells are affected.
Early and accurate diagnosis is key, as it determines the treatment and outcome of thymoma.
Clinical and pathological predictors, such as tumour size, histology, cancer stage, microscopic invasion and the presence of metastatic disease, are essential for prognosis and treatment planning of thymoma.
A complete resection, if possible, improves survival across all stages, underscoring the importance of surgical expertise in the treatment of thymoma.
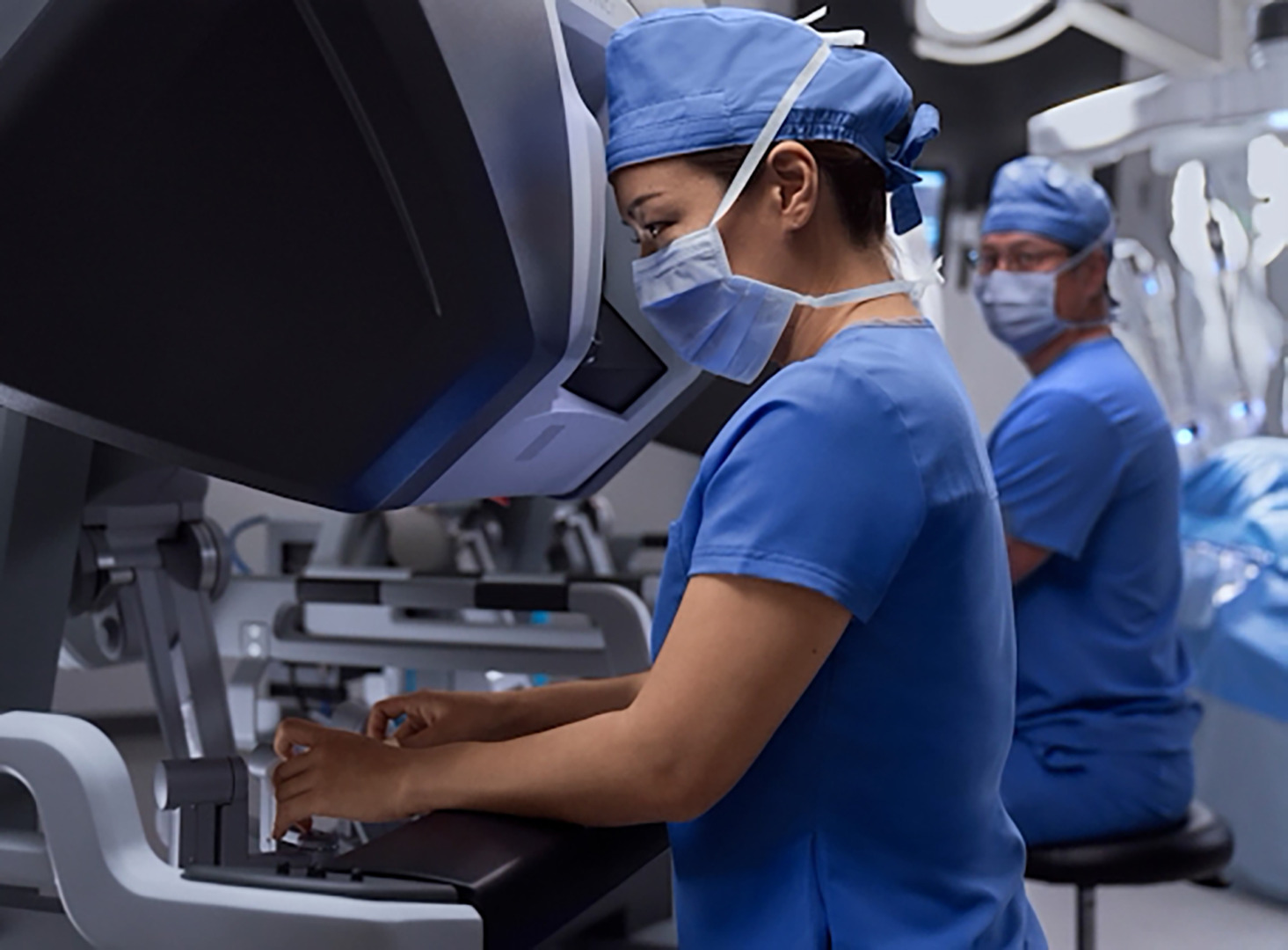
Thymoma treatment and cancer treatments have evolved significantly. Standard treatment to treat thymoma may include surgery, radiation therapy, chemotherapy, targeted therapy, and hormone therapy. The common treatment approach depends on the cancer stage and whether the thymoma or thymic carcinoma can be completely removed.
These minimally invasive approaches are ideal for early-stage thymomas, in which complete removal can be curative. Larger or more invasive tumours may require open thymectomy. The surgical goal is to achieve complete resection with clear margins.
For advanced or malignant thymomas, surgery may be combined with cancer treatments like radiation or chemotherapy to destroy the cancer cells effectively. Targeted therapy and hormone therapy can also be used to attack cancer cells in advanced thymomas.
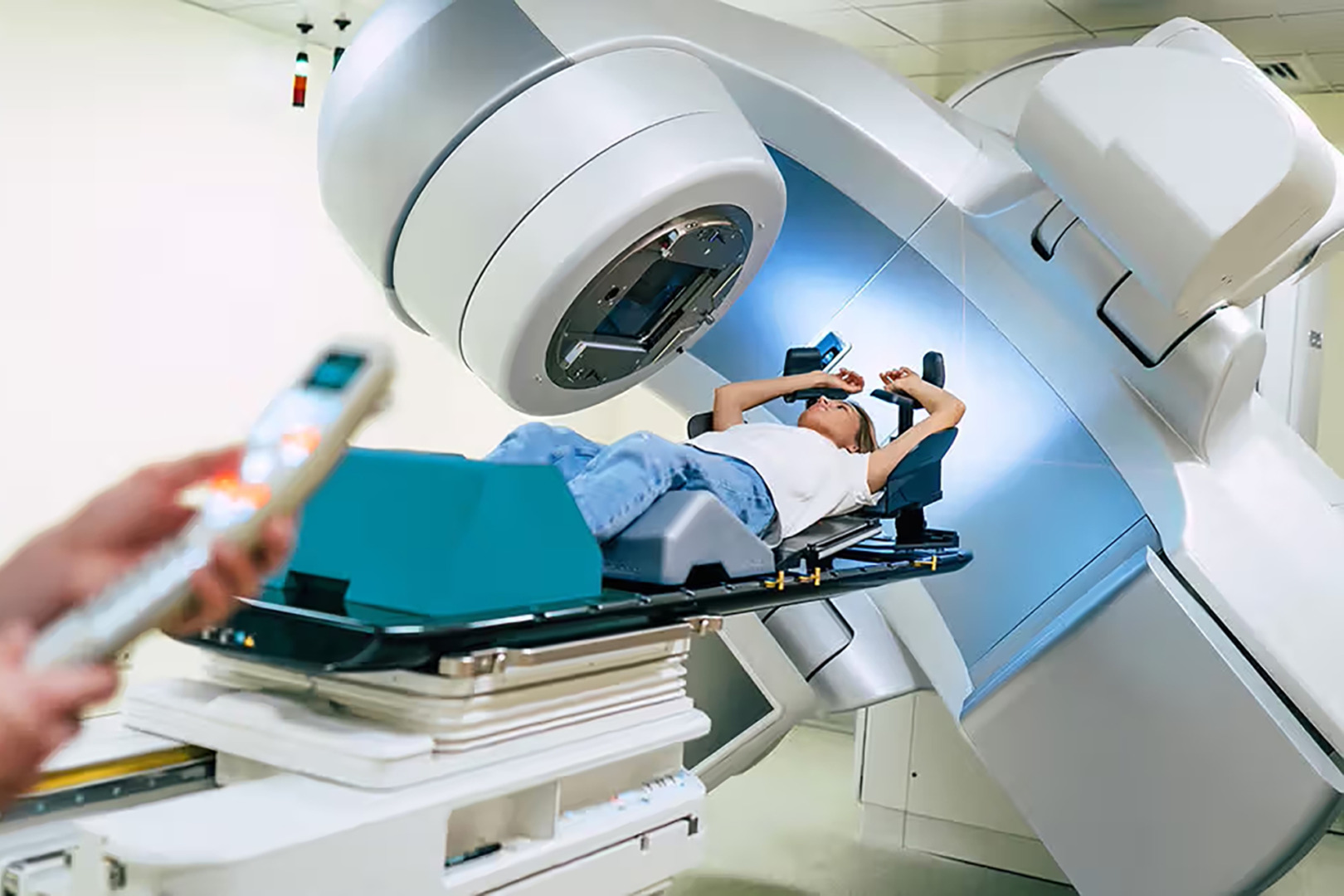
Radiation therapy and adjuvant radiotherapy play an important role in thymoma treatment, especially after an incomplete resection. A radiation oncologist will guide the precise dose delivery while minimising exposure to the heart, lungs and other critical structures.
For patients with inoperable disease due to an extensive invasion or medical contraindication to surgery, radiation therapy can be used as the primary treatment. While not as effective as a complete surgical removal, radiation can provide local control and symptom relief in carefully selected cases.
Chemotherapy has multiple roles in comprehensive thymoma treatment. Neoadjuvant chemotherapy, given before surgery, can shrink large tumours and facilitate complete resection. This is particularly useful for bulky Stage III thymomas or for cases in which the initial assessment suggests borderline resectability.
Adjuvant chemotherapy given after surgery works to target any remaining microscopic disease. This is typically reserved for high-risk cases with incomplete resection or aggressive histologic features. Common chemotherapy regimens combine platinum-based drugs with other agents like doxorubicin or etoposide.
For metastatic or recurrent disease, systemic chemotherapy is the primary treatment option. Chemotherapy regimens are designed to kill cancer cells throughout the body. However, thymic carcinomas may require more aggressive treatment regimens.

As with many cancers, early detection improves treatment outcomes. When caught early, benign thymomas can be cured with surgery alone, while malignant thymomas are more responsive to a combination of therapies.
Thymoma management, especially if malignant, requires a multidisciplinary approach. Early detection gives thoracic surgeons, oncologists and radiologists more time to develop and administer a personalised cancer treatment plan that considers the tumour stage, the patient’s overall health, and potential complications.
Neumark Lung & Chest Surgery Centre focuses on providing comprehensive care with the latest technology and a patient-centred approach. From diagnosis to advanced surgical techniques, we prioritise early detection, accurate staging and minimally invasive treatment to get the best results.
Follow-up care is essential for anyone being treated for thymoma or thymic carcinoma, as these rare cancers can recur even after initial therapy. Regular appointments allow for close monitoring, early detection of any recurrence, and prompt management of new or persistent symptoms.
Imaging studies, such as CT or PET scans, are commonly used to track changes or identify new growths. Blood tests can also provide insight into the immune system’s health and detect potential complications. Long-term effects of treatment, particularly radiation therapy, need to be monitored and managed.
Overall health and well-being are a key part of follow-up care. This includes managing any ongoing symptoms, staying up to date with recommended screenings and seeking support for emotional and psychological needs.
The prognosis and survival rate for thymoma patients vary greatly depending on the stage and type of cancer. Generally, thymoma’s 5-year survival rate is very good, at 80-90%, though the answer differs between thymoma and thymic carcinoma. The latter is a more aggressive cancer and has a 5-year survival rate of 50-60%. These rates depend on factors such as the type and stage of cancer, the patient’s overall health, and the response to treatment. Early detection, timely intervention, and the assistance of thymoma cancer specialists are key to improving the prognosis and survival for anyone with thymoma or thymic carcinoma.
Whether benign or malignant, thymomas require specialised care and a personalised approach. Minimally invasive procedures like RATS and VATS offer new ways of handling thymomas, giving patients hope and a better quality of life.
If you or a loved one has been diagnosed with thymoma or is experiencing concerning symptoms, don’t wait. Contact Neumark Lung & Chest Surgery Centre today to book an appointment. Early detection and specialised care can save lives and give you clarity, relief and direction.
A true thymoma is not usually regarded as a benign lump. Some thymomas are slow-growing and may stay localised for a long time, but they can still invade nearby tissue or recur later. Benign conditions can occur in the same area, such as thymic cysts, but those are different from thymoma.
Non-invasive types like Type A and AB often do not require any further treatment following complete surgical removal. However, more aggressive subtypes, such as B2 or B3, carry a higher risk of recurrence. In these cases, particularly if the surgeon notes the tumour has invaded neighbouring structures, post-operative radiotherapy is commonly recommended to sterilise the area and significantly reduce the chance of the cancer returning.
Surgery often improves but does not reliably cure the associated myasthenia gravis (MG). MG is an autoimmune condition, and removing the thymus (thymectomy) can induce long-term remission in many patients, even if the thymus gland itself does not harbour a tumour. When a thymoma is present, its removal is still mandatory. In fact, many patients with thymoma see an improvement in their MG symptoms post-surgery, though they will usually require continued medical management by a neurologist.
Minimally invasive approaches, such as VATS (Video-Assisted Thoracic Surgery) or RATS (Robotic-Assisted Thoracic Surgery), can still be safely used for larger thymoma treatments, provided the surgeon can achieve an R0 resection (complete removal with clear margins) if the tumour is large but shows no signs of invading major blood vessels or the lung, a robotic approach offers superior visualisation and precision for meticulous dissection. The decision hinges on the ability to achieve a complete, clean removal, not simply the tumour’s size.
Yes, absolutely. Recurrent thymoma often appears locally (in the chest) and usually grows slowly. If the recurrence is limited to one or two accessible sites, surgery is frequently preferred again, even after a prior operation or radiotherapy. The surgeon’s aim is once more to remove all gross disease. The patient’s overall health and previous treatment history will determine if surgery is followed by further chemotherapy or radiotherapy.
Thymoma can be serious, but it is not automatically fatal. Many thymomas grow slowly, and outcomes are often better than thymic carcinoma, especially when the tumour is found early and can be removed completely. Prognosis depends mainly on the stage, whether surgery can remove it entirely, and whether it has spread or recurred.
Yes, many people do live with a thymoma during diagnosis, treatment, and follow-up. Even so, it should not be ignored because it can grow, press on nearby structures, or return after treatment.
DISCLAIMER: The information provided on this website is for general informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. The use of this website does not create a doctor-patient relationship and no medical advice should be inferred or assumed. It is the user’s sole responsibility to seek the advice of their healthcare professionals for any medical concerns they may have and the user should not disregard, or delay, prompt medical advice for any such condition.
Neumark Lung and Chest Surgery Centre benefits from the expertise of a multidisciplinary team led by Dr Harish Mithiran, senior consulting thoracic surgeon at Gleneagles Hospital and Mt Alvernia Hospital.
Neumark is a lung and chest specialist centre with access to leading treatment modalities to achieve the best possible outcomes for lung disease and preventative patient screening.
Our foremost priority is to treat your condition as effectively as possible. Schedule a private consultation today; complete the form below, call, +65 6908 2145; WhatsApp, +65 9726 2485; or email, info@neumarksurgery.com.
Gleneagles Medical Centre
6 Napier Road
#02-09 Gleneagles Medical Centre
Singapore 258499
Mount Alvernia Hospital
820 Thomson Road
#06-07 Medical Centre A
Singapore 574623