What Is Combined Small Cell Lung Carcinoma?
Combined small-cell lung carcinoma (C-SCLC) is a rare and aggressive form of lung cancer. What makes it distinct is that it is a mix: the aggressive small cell lung cancer (SCLC) is found together with one or more types of non-small cell lung cancer (NSCLC) within the same tumour. The small cell carcinoma combines the aggressive nature of small cell lung cancer with the traits of the non-small cell carcinoma, and getting an accurate diagnosis and creating a careful, coordinated treatment plan are absolutely necessary.
This combined small-cell tumour is multiphasic, meaning it comprises multiple histologic cell types. It must contain confirmed SCLC cells mixed with at least one other NSCLC cell type. The non-small cell component could be squamous cell carcinoma, lung adenocarcinoma, large cell carcinoma, or, less often, large cell neuroendocrine carcinoma. In extremely rare cases, a giant cell carcinoma component may also be present.
This difference is crucial because the treatment plan for small cell lung cancer is based on the complete picture of the cancer cells, including both the SCLC and NSCLC elements.
When the tumour is pure SCLC, the usual first-line treatment involves drugs through systemic chemotherapy and radiation therapy. However, if the tumour also contains a NSCLC component, additional options may become available. These options may include surgical resection to remove the lung mass and, in some cases, newer treatments such as targeted therapy or immunotherapy. These newer treatments target specific changes, such as EGFR mutations that may be present in the non-small-cell component of the tumour.
Prevalence and Cancer Statistics
It is estimated that combined SCLC accounts for approximately 2% to 28% of all small cell lung cancer cases. However, the actual number of lung cancer cases is probably higher. This is because small biopsy samples do not always capture the full picture. Many cases of combined small cell carcinoma are correctly identified only after surgery, when the entire tumour is removed as a surgical specimen and examined, revealing a mixture of histologic components that a small needle or scope biopsy might have missed.
Pure SCLC carries a poor prognosis, with a five-year survival rate that remains low. However, the survival rate for combined small-cell lung carcinoma may be somewhat better when diagnosed at an early stage, particularly at Stage I. Combined small-cell lung carcinoma patients treated with a multimodal approach that includes surgery tend to have improved outcomes. The prognostic significance of the NSCLC element within the tumour is an active area of research.
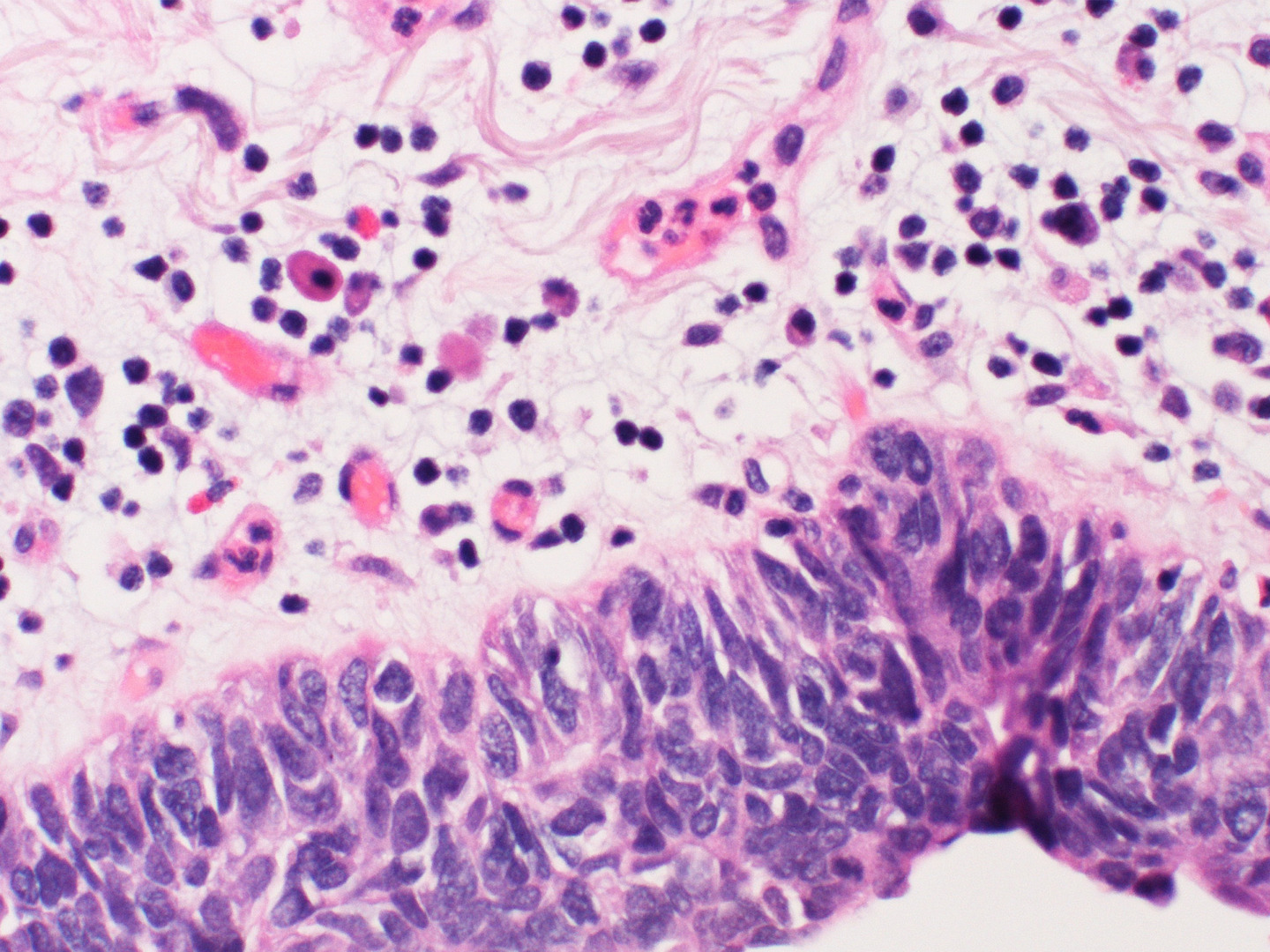
Histological Classification
Combined small-cell lung carcinoma is defined by the presence of different histological components within the same lung mass. The small cell carcinoma component must be present alongside at least one non-small cell cancer element. Genotypic and immunophenotypic analyses of surgical specimens help confirm the diagnosis. The most commonly observed non-small cell components include:
- Adenocarcinoma: Adenocarcinoma may harbour EGFR mutations, including cases with the same EGFR mutation as pure lung adenocarcinoma. Pulmonary adenocarcinoma within C-SCLC may respond to targeted therapy.
- Large cell carcinoma: A less-differentiated component of NSCLC. In extremely rare cases, giant cell carcinoma may also be found within a combined small-cell specimen.
- Squamous cell carcinoma: Lung squamous cell carcinoma is one of the most frequently identified NSCLC components in combined small cell lung tumours. Squamous cell carcinoma within a combined small cell tumour may exhibit clinical characteristics distinct from those of pure squamous cell lung cancer.
Immunohistochemistry is essential for identifying the small cell component. Negative staining for small cell markers in certain areas of the tumour, combined with positive staining in other areas, confirms the presence of separate histological components.
Symptoms and Warning Signs
The signs and symptoms of combined small-cell lung carcinoma are very similar to those of other lung cancers. The most common things people report include:
- A cough that will not go away
- Difficulty breathing or feeling short of breath
- Chest pain
- Losing weight without trying
- Feeling very tired
- Coughing up phlegm that has streaks of blood in it
Because SCLC often originates in the main airways, it can cause obstruction early on. This can lead to frequent bouts of pneumonia, difficulty breathing or wheezing that do not get better with standard asthma treatments. A lung nodule discovered on routine imaging may be the first sign of lung cancer. In some SCLC patients, a lung mass may grow rapidly and cause a pleural effusion, a buildup of fluid around the lung.
Certain warning signs mean you should seek urgent medical attention:
- Sudden and significant worsening of breathlessness or difficulty breathing
- New or persistent coughing up of blood (haemoptysis)
- Hoarseness that lasts longer than three weeks
- Unexplained swelling in the face or neck, which may indicate a blockage in the superior vena cava
- Pleural effusion causing increasing shortness of breath
If you are a current or former smoker and have any combination of these symptoms, you should get a quick evaluation from a specialist.

Causes and Risk Factors
Smoking is the main risk factor for both regular SCLC and C-SCLC. While most patients have smoked heavily, it can also extremely rarely occur in people who have never smoked. Exposure to workplace carcinogens such as asbestos, radon and certain heavy metals over extended periods can further increase this risk.
Scientists believe that C-SCLC arises from a specialised cancer cell type that can differentiate into multiple tissue types. This cancer cell becomes cancerous and then divides into two distinct lineages, producing both SCLC and NSCLC within the same tumour.
Genetic analysis shows that both tumour parts typically share the main mutations in SCLC (TP53 and RB1), but they also acquire distinct secondary mutations. This ability of a cancer cell to change its identity, known as ‘lineage plasticity’, is a major focus of research. It may explain why some NSCLC tumours, particularly EGFR-mutant adenocarcinomas treated with certain targeted drugs, can transform into SCLC.
Diagnosis in Singapore
To obtain an accurate diagnosis of C-SCLC, physicians require sufficient tissue for expert review. Although a small sample obtained during a procedure such as bronchoscopy or CT-guided needle aspiration can confirm small cell lung cancer, it may not include the NSCLC component. Small samples from these lung tumours can also be difficult to interpret due to ‘crush artefact’, or damage to the cancer cells that happens during the biopsy.
For many SCLC patients, the definitive diagnosis is only confirmed after a surgeon removes a larger tissue sample that can be thoroughly analysed using specialised laboratory tests.
At Neumark, doctors usually start checking for lung cancer with a CT scan of the chest that uses a special dye. This is followed by a PET/CT scan to assess the extent of disease spread (staging).
If a sample of the lymph nodes in the centre of the chest is needed, Dr Harish Mithiran of Neumark Lung & Chest Surgery Centre organises a procedure called bronchoscopy with endobronchial ultrasound-guided biopsy.
If the first tissue sample suggests a SCLC, but scans or the patient’s general health suggest it might be a mix of cancer types, the care team may suggest a surgical biopsy or early tumour removal. This helps get a clear diagnosis of a C-SCLC.
Specialised lab tests on the tissue, called immunohistochemistry, are key. Markers like synaptophysin, chromogranin A, and CD56 confirm the presence of the SCLC component. Negative staining for these markers in other areas helps identify NSCLC components. Other markers, such as TTF-1, p40, and napsin A, help identify the NCLC part. Testing tumour genes for EGFR mutations and ALK rearrangements through genetic analysis is increasingly important, particularly when adenocarcinoma is present.
These genetic findings can affect the outlook for SCLC patients and help doctors choose the best treatment for lung cancer.
Combined Small Cell Lung Carcinoma Treatment
There is no single standard approach to treating C-SCLC. Instead, medical teams need to collaborate to develop a personalised plan for patients with C-SCLC, considering several important factors, including the extent of cancer progression, the proportion of the tumour that is NSCLC-type, the cancer cell genetic profile, and the patient’s overall health. Treatment for C-SCLC draws on approaches used for both SCLC and NSCLC.
Chemotherapy
The main first-line treatment for C-SCLC is usually combined chemotherapy, typically including platinum-based drugs and etoposide. This combined chemotherapy approach is often the first-line treatment for lung cancer that has spread.
For extensive disease, doctors may also add treatments that use the body’s immune system to fight lung cancer (immune checkpoint inhibitors, like atezolizumab or durvalumab). Adding these to chemotherapy has been shown to improve how long people with pure SCLC live and is often considered for C-SCLC as well.
If the NSCLC component of lung cancer has a specific alteration, such as EGFR mutations or ALK gene rearrangements, targeted drugs may be used. These may be administered after the initial treatment ceases to work, or in combination with chemotherapy.
Radiation Therapy
Radiation therapy is a key part of treatment for early-stage SCLC. Radiation therapy involves using high-powered energy beams to kill cancer cells, often applied along with chemotherapy, to the main tumour and the lymph nodes in the chest.
To reduce the risk of SCLC spreading to the brain, doctors may also discuss a treatment called prophylactic cranial irradiation (PCI). This is a type of radiation therapy administered to the brain, in accordance with standard guidelines for the management of SCLC.
Surgery
Combined small cell lung carcinoma may be diagnosed at an operable stage more often than pure small cell lung cancer in some patients. For carefully selected SCLC patients and C-SCLC patients with localised disease and absent or limited lymph node involvement, surgical resection, followed by chemotherapy and radiotherapy, may be associated with better outcomes than drug therapy alone. Studies confirm that surgical resection at Stage 1 can improve the survival rate for combined small cell lung carcinoma.
When lung cancer surgery is appropriate, minimally invasive techniques such as VATS or RATS may be used to perform a lobectomy or segmentectomy through small incisions, which can reduce pain and support a quicker recovery than open surgery. The choice of approach depends on the size and location of the lung mass (e.g., upper lobe), lymph node involvement, lung function, and overall health.
Open surgery or non-surgical treatment may be preferred for large or central lung tumours, dense scar tissue, or significant mediastinal lymph node disease. Risks include bleeding, infection, pneumonia, prolonged air leak, and the possibility of conversion to a thoracotomy if needed for safety.
At Neumark, Dr Harish Mithiran performs thoracic surgery at Gleneagles Hospital on Napier Road and at Mount Alvernia Hospital on Thomson Road, providing patients in Singapore with convenient access to specialist surgical care for lung cancer.
Prognosis and Outlook
The prognosis for combined small cell lung carcinoma depends on the stage at diagnosis and the proportion of the small cell component. C-SCLC patients diagnosed at Stage 1 who undergo surgical resection may have a better survival rate than SCLC patients treated with chemotherapy alone. Pure SCLC diagnosed at an advanced stage carries a very unfavourable prognosis.
Cancer research suggests that the clinical features of the non-small cell component may influence outcomes in patients with C-SCLC. The prognostic significance of specific molecular markers and other alterations is also under investigation. Further cancer studies and thoracic cancer publications are needed to establish definitive treatment guidelines for each histological variant of combined small cell lung carcinoma.
Recovery and Follow-Up
If you have minimally invasive lung surgery for SCLC, you can generally expect to stay in the hospital for two to five days. Most people return to light activities within 2 to 3 weeks and can resume more challenging physical tasks within 1 to 2 months.
If you have open chest surgery, recovery typically takes longer. You will likely stay in the hospital for five to seven days and will need more time to get back to your full daily routine.
After the surgical removal of the tumour, doctors usually recommend chemotherapy. This additional treatment is called adjuvant therapy and is given to help kill any remaining cancer cells that may have spread, which is a high risk with this type of small cell lung cancer.
Your follow-up care will include regular CT scans and doctor visits to monitor your progress. In some cases, you may also have an MRI scan of your brain. The care team at Neumark, which includes doctors from different specialities, will work closely together to manage this schedule. They will adjust your plan based on the tumour’s lab results, any specific molecular findings, and your body’s response to treatment.
It is important to note that the small-cell cancer component tends to recur, often within the first two years. Pleural effusion, new lung nodules, or recurrent breathlessness should be evaluated promptly. Adhering to your surveillance schedule and seeking prompt treatment at the first sign of recurrence are essential to achieving optimal health outcomes.

Why Choose Neumark?
At Neumark Lung & Chest Surgery Centre, a team specialising in chest and lung care, including experienced chest surgeon Dr Harish Mithiran, provides coordinated treatment. For complex diagnoses such as c-SCLC, this multidisciplinary team approach, involving surgery, oncology, radiology and pathology, ensures a carefully tailored treatment plan.
If you have been diagnosed with SCLC or a mixed lung cancer type, prompt specialist consultation is crucial. Contact Neumark Lung Cancer Treatment Centre to consult Dr Harish Mithiran at Gleneagles or Mount Alvernia hospitals. Our team provides clear treatment options and compassionate guidance for patients with lung cancer.

